- The majority of cardiorespiratory arrests in infants and children are secondary to hypoxaemia and/or hypotension. However, it is important to recognise that Sudden Cardiac Arrest can also be seen in young people, due to dysrhythmias caused by underlying channelopathy, cardiomyopathy or myocarditis. Up to 25% of these cases have shockable rhythms.
- This CPG refers to patients generally 3 hours old to 12 years of age.
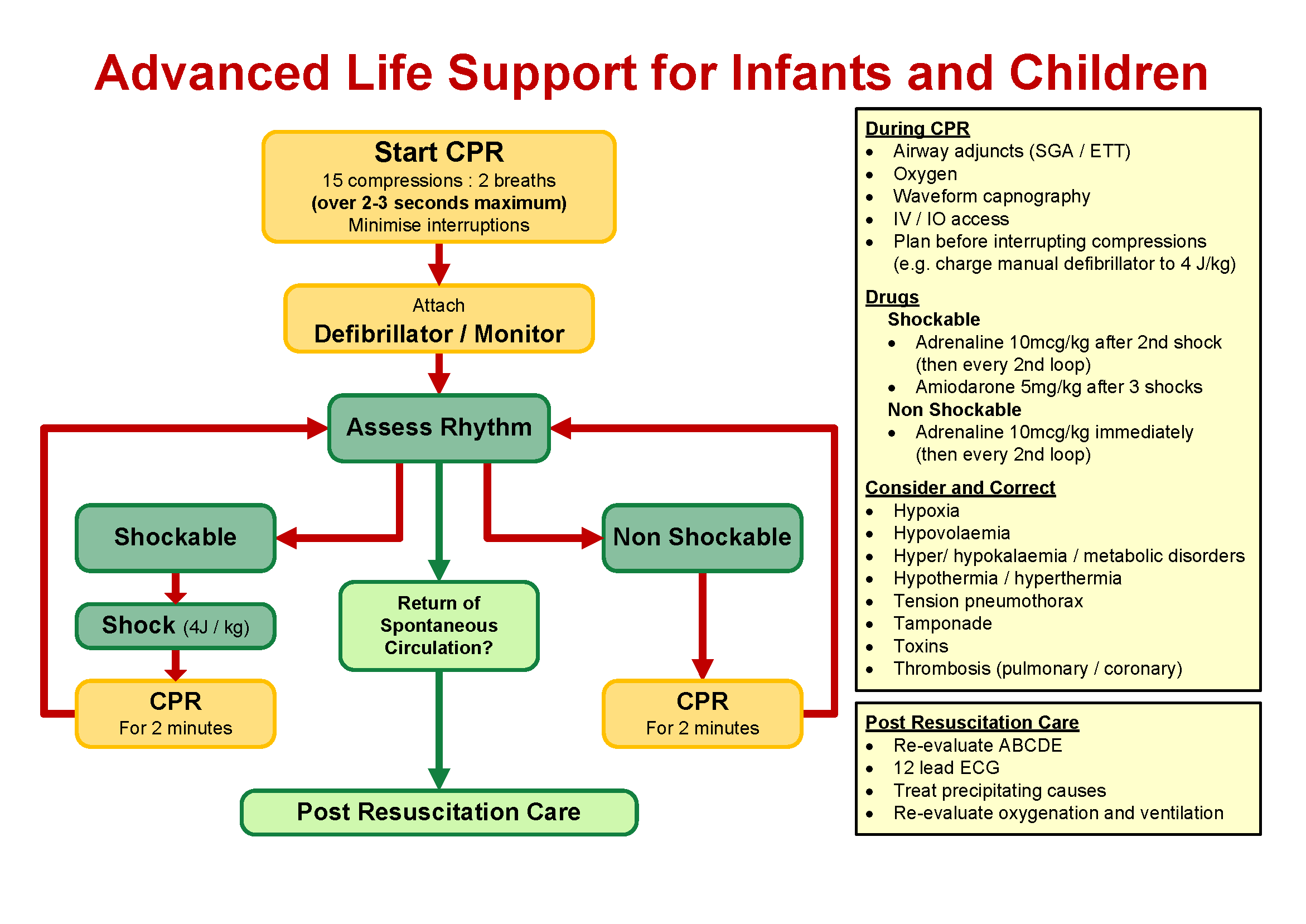
- Cardiac arrest is a time critical condition requiring immediate intervention. The ALS algorithm allows for a systematic approach to cardiac arrest and assumes basic life support (BLS) measures have been initiated and remain ongoing.
- Respiratory arrest may occur alone, but if treated promptly may not progress to cardio-respiratory arrest.
- Respiratory arrest with adequate cardiac output should be treated as per post resuscitation care.
- Bradycardia is an ominous sign in the infant / paediatric patient. If their pulse is <60bpm, they are unconscious AND display signs of poor perfusion, commence CPR.
- If circulation is restored, refer to Return of Spontaneous Circulation (ROSC) CPG.
- Following a primary survey, resuscitation must be commenced on all patients in suspected cardiac arrest not meeting the criteria set out in the Determination of Death (TOR/ROLE) CPG, in line with Australian Resuscitation Council (ARC) guidelines.
- If trauma is the cause, follow the Traumatic Cardiac Arrest CPG.
- Consider early transportation for non-asystole patients as they will not meet the clinical criteria for termination of resuscitation efforts.
- Ensure appropriate padding for neutral alignment to open the airway.
- Effective airway control and adequate ventilation with oxygen supplementation are the keys to favourable outcomes in infants and children.
- If vascular access is unobtainable, continue resuscitative efforts without medications
- Calculations are based on weight in kilograms; use the Paediatric Drug Calculator
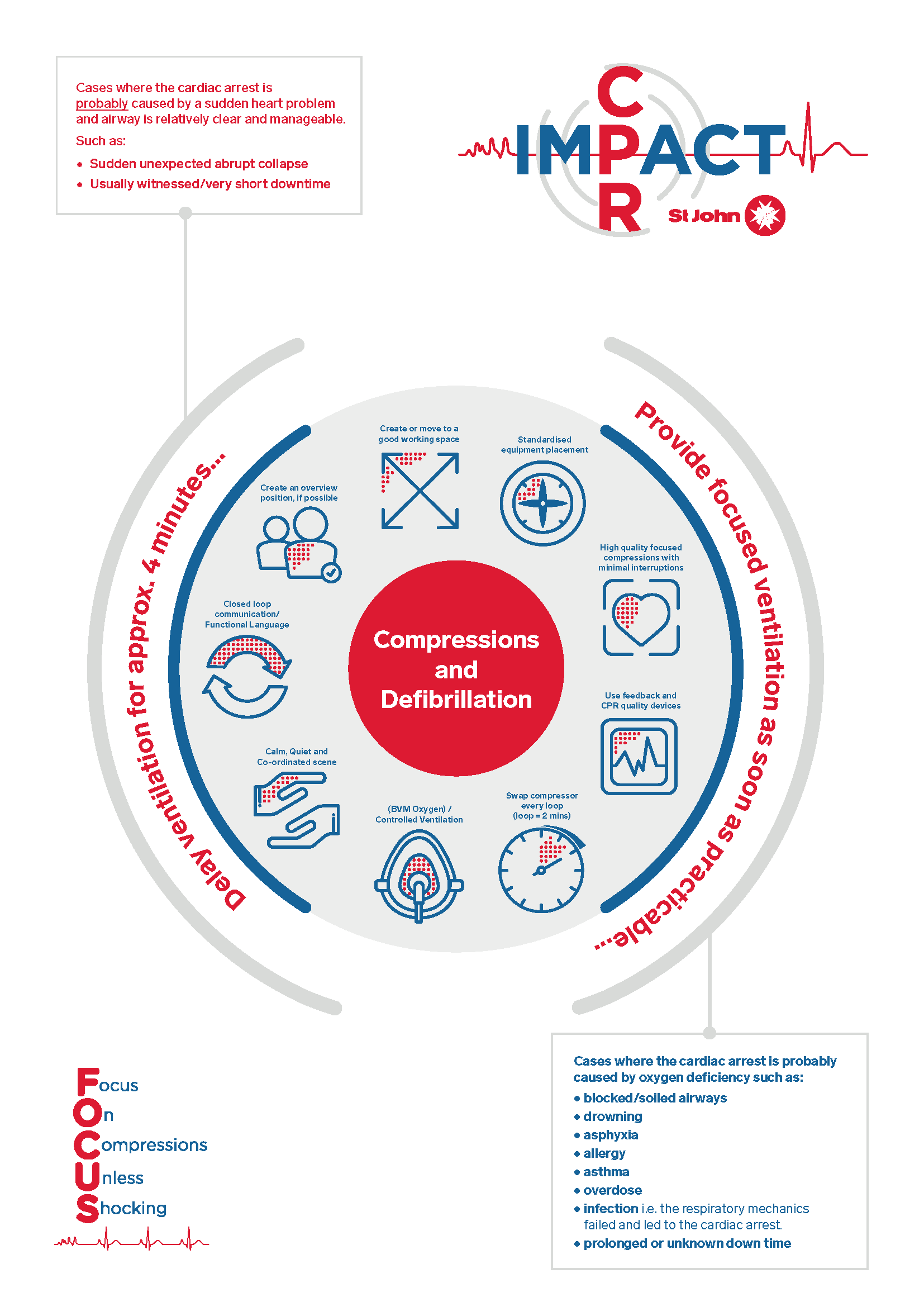
The treatment for Cardiac Arrest patients revolves around core requirements; excellent quality chest compressions that are never interrupted unnecessarily, timely defibrillation and oxygenation.
Traditionally, these care needs have been approached in a regimental manner, and often some skills are prioritised at the expense and quality of others. Prioritising the core elements is essential and apply each of the other principles around that as necessary – as soon as it is possible to do so.
There is no prescribed order for this; it is dynamic and circumstance dependant as reflected in the Circular Diagram below.
| Working space | Good resuscitation cannot generally be delivered in poor environments. A rapid and dynamic risk assessment should be done to either create space or move the patient. |
| Standardised equipment placement | The right equipment in the right place as often as possible. |
| High quality compressions | Focused compressions (attention to quality) that are minimally interrupted. The use of CPR Quality Feedback Devices (where available) is mandatory. |
| Swap compressor EVERY 2 MINUTES | A fatigued compressor delivers poor quality compressions. Prioritising paramedic skills over a swap of compressor in resource poor cases should not routinely occur unless it is critical to do so. |
| Create overview | Scene leadership should be established as soon as practicable. This person should NOT be delivering skills, and ideally be standing away. |
| Maintain a calm, coordinated scene | Encourage a calm and controlled scene with closed loop communication between the team, using functional language. |
| Ventilation | The use of a BVM should be viewed as an important task in providing controlled ventilation. Aim for correct rate without excessive volumes under pressure. |
Commence High Quality, Task Focused, Minimally Interrupted Chest Compressions.
- Assess & defibrillate "shockable" rhythms every 2 minutes safely with a minimal peri-shock pause (follow prompts if using AED).
- Shockable Rhythms: VF, Pulseless VT; 4 joules per kg.
- Non-Shockable Rhythms: PEA, Asystole.
- Clear airway and oxygenate patients early via controlled BVM ventilation as soon as practicable. Do NOT passively oxygenate children
- Do not perform asynchronous ventilation
- Work as a team, communicate well and establish a 'hands-off' overview position.
- Apply CPR Feedback Device to monitor and correct CPR performance
- Corpuls CPR Feedback Device: ≥ 6 years old or 20kg
- Q-CPR Feedback Device: ≥ 8 years old or 25kg (Some AED's still have Q-CPR)
- As per Primary Care guidelines
- Insert supraglottic airway devices
- Once a supraglottic airway is in-situ (including i-gel), maintain a 15:2 regimen (this aids in situational awareness and control)
- Asynchronous ventilation is not recommended in paediatric cardiac arrest
- Obtain vascular access when possible to do so.
- Adrenaline as per CPG after 2nd shock (or ASAP after IV access has been established) and thereafter every 2nd loop.
- Amiodarone after a total of 3 shocks have been given (including AED shocks delivered prior to ambulance arrival).
- Fluid therapy as per CPG for hypovolemic cardiac arrest
- Glucose as per CPG in suspected hypoglycaemic cardiac arrest
- Do not attempt endotracheal intubation where a supraglottic device is adequate
- Hypothermia in Western Australia as a cause of cardiac arrest is extremely rare and mostly accidental e.g. locked in a cool room. If you suspect that the cardiac arrest was secondary to hypothermia, the emphasis is on high performance CPR and transport.
- ASMA available for advice.
- Refer to Determination of Death (TOR/ROLE)
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.