
- Effective hand hygiene is widely recognised as the single most important strategy for the prevention of healthcare associated infections.
- Effective hand hygiene reduces or inhibits the growth of microorganisms and prevents the transmission of pathogens between patients and healthcare workers
Hand Hygiene is a general term referring to any action of hand cleansing. There are three ways hand hygiene can be performed:
- Applying a waterless antimicrobial hand rub to the surface of the hands e.g. alcohol based hand rub (ABHR).
- Washing hands with the use of a water and soap or a soap solution, either non-antimicrobial or antimicrobial.
- Use of the approved hand wipes
ABHR is gold standard for hand hygiene for all clinical situations where hands are visibly clean.
Wash with soap and water when hands are visibly dirty, when visibly soiled with blood or other body fluids, or when caring for patients with symptoms of gastroenteritis.
When there is no readily available access to hand washing facilities, the approved hand wipes can be used. It is recommended to wash hands with soap and water as soon practical.
Five Moments for Hand Hygiene have been identified as the critical times when hand hygiene should be performed to protect:
- Patients against acquiring infectious agents from the hands of healthcare workers
- Patients from infectious agents (including their own) entering their bodies during procedures
- Healthcare workers and the healthcare environment from acquiring patients’ infectious agents
“5 Moments for Hand Hygiene (Adapted by the Council of Ambulance Authorities)”
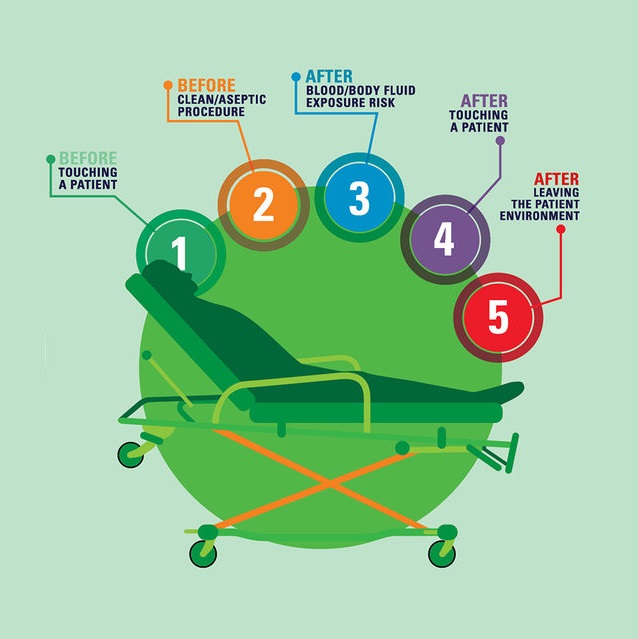
| Moment 1: | Examples: |
|---|---|
Before Touching A Patient When Perform hand hygiene on entering the patient zone before touching the patient Why To protect the patient against acquiring harmful micro-organisms from the hands of the healthcare worker |
|
| Moment 2: | Examples: |
Before a Procedure When Immediately before a procedure. Once hand hygiene has been performed, nothing else in the patient's environment should be touched prior to starting the procedure Why To protect the patient from harmful micro-organisms from entering their body |
|
| Moment 3: | Examples: |
After a Procedure or Body Fluid Exposure When Hand hygiene immediately after a procedure or body fluid exposure risk as hands could be contaminated with body fluid Even if you have had gloves on you should still perform hand hygiene after removing them as gloves are not always a complete impermeable barrier. Hands may also have been contaminated in the process of removing the gloves. Why To protect the healthcare worker and the environment from becoming contaminated by the transmission of potentially micro-organisms from the patient |
|
| Moment 4: | Examples: |
After Touching a Patient When After touching a patient. Perform hand hygiene before you leave the patient zone. Why To protect the healthcare worker and the environment from harmful micro-organisms |
|
| Moment 5: | Examples: |
After Leaving the Patient's Environment When Hand hygiene after touching surroundings in the patient zone even when the patient has not been touched. Always perform hand hygiene before leaving the patient zone, and/or entering the healthcare worker zone. Why To protect yourself and the healthcare surroundings from becoming contaminated with potential organisms from the patient’s surroundings. |
|
It is recognised in the pre-hospital setting there may be times in emergency situations where hand hygiene is secondary to patient safety, however once the risk has been resolved further deviation is not warranted.
The Council of Ambulance Authorities has developed guidance for the zones of hand hygiene in the pre-hospital setting to determine when hand hygiene is needed. Performing hand hygiene when moving between zones will minimise the risk of contamination of patient care equipment and areas of the ambulance, and reduce cross contamination between patients and Ambulance personnel.
Patient zone (red zone)Includes the patient and the patient’s immediate surroundings. It is considered to be anywhere the patient can touch. |
Healthcare worker zone (yellow zone)Includes the healthcare workers immediate zone and where medical devices or consumables are placed while attending to the patient (e.g. monitor, treatment bags) |
Clean healthcare worker zone (green zone)Includes all nonpatient areas (e.g the front of the cab when transporting a patient, all of the vehicle post clean) |
Prior to departure
An ambulance or transport vehicle is considered a Clean Health Care Worker Zone (green) when entering to attend a case. Always perform hand hygiene prior to entering a Clean Health Care Worker Zone (your vehicle). Hand hygiene prior to entering this area ensures there is no cross contamination from your previous activities to your clean area, and your patient.
On scene
A patient’s house, or the area they are located is considered a Patient Zone (red). Perform hand hygiene when entering these areas to protect patients from transmission of pathogens on your hands. After touching the patient zone, perform hand hygiene prior to touching any response kit equipment or defibrillator in order to reduce cross contamination to your Healthcare Worker Zone. Perform hand hygiene when leaving the Patient Zone to prepare for departure.
During transit
The front of the vehicle is considered a Clean Healthcare Worker Zone (green) and typically shouldn’t contain infectious pathogens. The Patient Zone (red) is considered contaminated and includes any devices attached to a patient or any surfaces they may have touched. Areas where healthcare workers access or where medical consumables or equipment is stored is considered a Healthcare Worker Zone (yellow). Hand hygiene must be conducted with any movement between these zones to prevent cross contamination for patient and staff safety.
At the hospital
The Patient Zone (red) is considered to be any area where the patient can touch or would have personal items, and should be considered contaminated. The Healthcare Worker Zone (yellow) is where medical equipment and consumables are stored. Hand hygiene between entering and departing these two areas is essential to avoid the contamination of the patient into the Healthcare Worker Zone and vice versa.
Following handover
Once a patient has left the vehicle, the entire back area is now considered a Patient Zone (red) and you will require hand hygiene upon entering and departing. This includes prior to applying and doffing gloves when cleaning and post cleaning the vehicle.
The front of the vehicle is still considered a Clean Healthcare Worker Zone (green) and hand hygiene prior to entering this area is still required.
Follow these steps in order to prevent cross infection between patients and improve staff safety.
Other opportunities to decontaminate hands include (but are not exclusive to):
- At beginning and end of shift
- Before and after removal of gloves and other PPE
- Before and after handling food
- Before and after smoking
- Before and after using the bathroom
- After performing respiratory hygiene/coughing into hands
- Any time hands are visibly contaminated
- After vehicle checking
- After patient equipment/stretcher contact
- After cleaning equipment/vehicle
- On entering (where practical) and leaving the Emergency Department
To minimise the possible barriers to hand hygiene
- Keep fingernails short (i.e. the length of the finger pad) and clean. Nail varnish, artificial nails, extenders or tips are not to be worn.
- Rings with ridges and stones must not be worn. A plain metal ring is acceptable.
- It is recommended for all operational personnel to be bare below the elbows however a wrist watch may be worn. The watch must be cleaned regularly and removed prior to washing hands with soap and water. It is advised that the watch be waterproof and made from a wipeable material, with a flat, smooth wrist band to minimise the risk of harbouring pathogens.
- Long sleeved jackets can easily become contaminated, and impede access to the wrist for hand hygiene. Long sleeved jackets must be removed, and sleeves shortened to mid forearm unless long sleeves are required as part of PPE such as the wearing of high visibility jackets, coveralls, helicopter paramedic uniform.
Hand/Skin Care
- Healthy intact skin is an effective barrier against infection. It is important to take of your hands by using the correct hand hygiene method.
- ABHR is recommended for routine hand hygiene, unless hands are visibly soiled.
- Use warm water and not hot for hand washing.
- Ensure hands are dried thoroughly after washing. Pat dry hands using a disposable paper towel.
- Regularly use a hand moisturiser to prevent drying and cracking of the skin.
- Cover cuts, abrasions and lesions with a water resistant, occlusive dressing and change as necessary whilst on duty.
Skin Irritation and Allergy
All clinical staff and volunteers are screened for skin irritation/conditions and latex sensitivity during the pre-employment interview process.
The main type of occupational skin irritation associated with hand hygiene is irritant contact dermatitis. Symptoms include dryness, irritation, itching, and sometimes cracking of the skin. Allergic contact dermatitis is rare and is due to an allergy from an ingredient in a hand hygiene product.
Report all skin conditions (e.g. dermatitis, allergic eczema, weeping lesions) to your line Manager and seek medical advice from GP or Specialist.
Staff who have skin conditions such as exudative lesions or weeping dermatitis should be removed from direct patient care until the condition resolves.
Refer to Skin Irritation flowchart, adapted from Occupational Dermatology Research and Education Centre flowchart for healthcare workers
| Report problem to your Manager and Safety Team |
|---|
|
| Good Skin Care Practice |
Use ABHR Reduce handwashing (unless hands visibly soiled) and use ABHR where possible. ABHR may sting hands if split/cracked. It does not mean you are allergic to it. At home, use soap substitutes where possible. Use Moisturiser Moisturise hands regularly while at work – before the start of the shift, during meal breaks and at end of shift. Moisturise hands regularly at home. |
| See GP or Attend a St John Health Clinic |
If the previous advice has not improved your skin integrity, you will need to assessed by a doctor:
|
| Referral to a Dermatologist |
| If there has still not been improvement, you may need a referral from your GP to see a dermatologist. You may be referred to a special clinic for patch testing. Patch testing is used to diagnose an allergy to something that your skin is coming into contact with. |
Key Terms & Links
Further Reading:
Council of Ambulance Authorities Take Five for Hand Hygiene Campaign https://www.caa.net.au/hand-hygiene-subpage
National Hand Hygiene Initiative https://www.safetyandquality.gov.au/our-work/infection-prevention-and-control/national-hand-hygiene-initiative
Occupational Dermatology Research and Education Centre http://www.occderm.asn.au/
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.