
| Donning | |
|---|---|
| 1. | Hand hygiene |
| 2. | Gown / coverall |
| 3. | Respirator (fit tested and checked) |
| 4. | Eye protection / Face shield (face shield recommended if high risk of splashes and sprays of blood and body fluids e.g. trauma, haemorrhage) |
| 5. | Gloves |
| Doffing | |
|---|---|
| 1. | Gloves |
| 2. | Hand hygiene |
| 3. | Gown / coverall |
| 4. | Hand hygiene |
| 5. | Eye protection / Face shield |
| 6. | Hand hygiene |
| 7. | Respirator |
| 8. | Hand hygiene |
1. Perform hand hygiene (hand sanitiser in field settings OR soap and water with hand sanitiser in clinic or hospital settings)

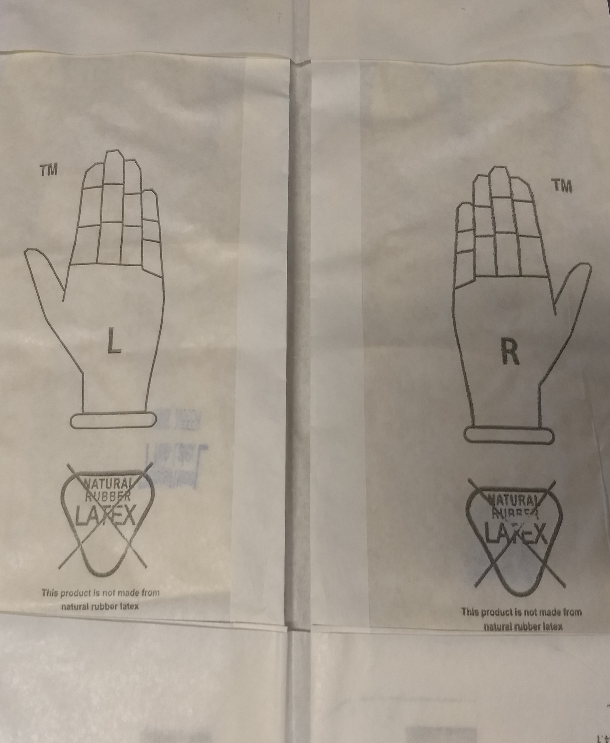
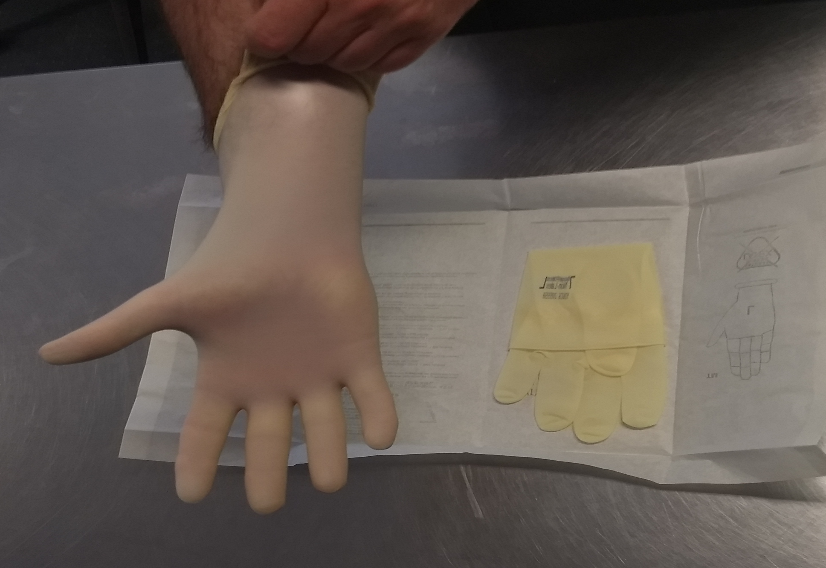
2. Select appropriate size gloves for wearer. Check package for integrity and use by date. If in doubt discard and get a new pair.




Non-clinical PPE (e.g. high-visibility jackets, helmets etc…) are not included in this document. Please refer to relevant Workplace Instructions and Safety information.
PPE includes:
- Nitrile gloves
- Surgical facemask
- P2/N95 respirator
- Protective eyewear or face shield
- Coveralls or Gowns
Nitrile Gloves
Gloves are worn as a barrier to protect the hands from contamination or to prevent the transfer of microorganisms already on the hands. They are single use items to be worn when performing invasive procedures, when in contact with non-intact skin or mucous membranes, and any activity where there is high risk of exposure to blood and body fluids, including cleaning of equipment and vehicles.
Gloves do not need to be routinely worn for all patient contact when the risk of exposure to blood and body fluids is minimal.
Prolonged glove use can lead to lack of hand hygiene and increase risk of contact dermatitis.
Hand hygiene must always be performed prior to donning gloves and immediately after removal (Refer to CPG 12.2. Hand Hygiene).
Surgical Mask
Surgical masks should be worn by the patient on droplet and airborne precautions to contain respiratory secretions of the wearer. They can also be worn by SJWA personnel as directed.
P2/N95 Respirator
P2/N95 respirator provides protection from diseases transmitted through the droplet and airborne route. P2/N95 respirators must be fit tested. A fit check must be performed before patient contact.
See Key Terms & Links for further instructions.
Indications for use of a P2/N95 respirator:
- Sprays of blood and body fluids likely (risk assessed as part of standard precautions)
- Droplet and airborne precautions
- During an aerosol generating procedure
- Patient with aerosol generating behaviours
- When cleaning large amounts of effluvia, blood or body fluid
- When required by a SJWA directive.
Indications for removal of P2/N95 respirator:
- P2/N95 respirator should be changed between patients and when they become damaged soiled or wet
- International guidance states that P2/N95 respirator can be continuously worn for up to 4 hours. Once they are removed they must be discarded and a new respirator used, if needed.
- P2/N95 respirator should never be reapplied after they have been removed.
- P2/N95 respirator should not be left dangling around the neck.
- The front of the respirator is likely to be contaminated therefore touching this area while wearing it should be avoided.
- Hand hygiene should be performed upon touching or discarding a used respirator.
Protective Eyewear
Protective eyewear protects the conjunctiva from exposure to blood, body fluids, and secretions propelled into the air by coughing or sneezing.
Reusable protective eyewear should be cleaned and disinfected following use.
Disposable full face shields and are recommended when there is a high risk of splashes and sprays of blood and body fluids (e.g. trauma, haemorrhage) and are to be discarded after use.
Prescription eyewear is not considered protective as it allows contaminants to travel between the lens and the face.
Indications for the use of protective eyewear:
- Sprays of blood and body fluids likely (risk assessed as part of standard precautions)
- Droplet and airborne precautions
- During an aerosol generating procedure
- Patient with aerosol generating behaviours
- When cleaning large amounts of effluvia, blood or body fluid
- When required by a SJWA directive.
Disposable Coveralls or Gowns
Disposable fluid-resistant coveralls or gowns are used to prevent skin and uniforms being contaminated with blood/ bodily fluids. The need for a gown/coverall will depend on the degree of risk, including the anticipated degree of contact with infectious material and the potential for blood and body substances to penetrate through to clothes or skin.
Indications for the use of coveralls/gowns:
- Sprays of blood and body fluids likely (risk assessed as part of standard precautions)
- Droplet and airborne precautions
- During an aerosol generating procedure
- Patient with aerosol generating behaviours
- When cleaning large amounts of effluvia, blood or body fluid
- When required by a SJWA directive
PPE not routinely recommended
The following items are not routinely recommended as part of contact, droplet or airborne precautions, however for specific situations may be introduced as a SJWA directive.
Head coverings
- Generally do not prevent the wearer from contamination.
- Add in an additional step in PPE doffing process therefore increase the risk of contamination of the wearer.
Boot covers
Use of boots covers is not recommended unless gross contamination is anticipated, as:
- Boot covers can pose safety risk due to the risk of slipping and self-contamination at removal.
- Boots should be made of material that can be cleaned and disinfected.
- Boots should be wiped over at the end of each shift with a cleaning and disinfectant agent.
- Boots should be left at the workplace, where practical or left outside the home.
Powered air-purifying respirators (PAPRs) are an alternative to P2/N95 respirators in selected circumstances:
- PAPRs require specific training and must only be used by personnel trained in their use, including safe removal with other PPE.
- Currently only the Special Operations Paramedics and selected staff who have been trained for the Specialised Isolations Ambulances, are able to use PAPRs.
Donning and Removal of Personal Protective Equipment (PPE)
To reduce the risk of transmission of infectious agents, PPE must be used appropriately. Ideally PPE should be applied before patient contact. In the pre-hospital setting it is not always possible to identify times when PPE is required and this will need to be assessed on the individual basis.
If it is suspected or confirmed the patient has an infection that can be spread by the droplet or airborne route (such as influenza, measles) place a surgical facemask on the patient to help minimise the spread of respiratory droplets. However not all patients will be able to tolerate this. In these cases, encourage the patient to use a tissue to cover their nose and mouth when coughing/sneezing.
Sequence for donning PPE
- Perform hand hygiene
- Gown/Coveralls
- Gown:
- Slide arms through the armholes and through the cuffs.
- Secure the top of the gown at the back of the neck with the ties, tape or Velcro
- Secure the waist ties
- Coveralls:
- Select the correct size of coveralls.
- Unfold and unzip the coveralls.
- Place each leg into the suit. Take care not touch footwear.
- Fit coveralls over the body and shoulders, and allow the hood to hang free at the back.
- Zip up the coveralls
- Gown:
- P2/N95 respirator
- Open the P2/N95 respirator by separating the edges
- Cup the respirator to your chin and place the straps over your head
- Conform the respirator to your face by pressing with your fingers across the bridge of the nose until it fits snugly
- A fit check must be performed prior to undertaking any clinical activity in which a P2/N95 respirator is required. Fit checks ensure that the respirator is sealed over the bridge of the nose and mouth and that there are no gaps in the seal between the respirator and the face:
- Check for air leaks by placing both hands above and below the respirator whilst exhaling without disturbing the fit of the respirator.
- If you can feel air escaping, you do not have a good facial seal. Re-adjust the respirator by shifting the position of the respirator up or down your nose bridge, remoulding the nose wire and checking respirator edges sit snugly against the face.
- After adjusting, repeat the fit check.
- Once you have no air leaks, you have an adequate seal and can proceed
- Eye protection/face shield
- If you wear prescription glasses, place the protective eyewear over your glasses.
- If eye protection fogs up, you do not have a good seal of your P2/N95 respirator – readjust.
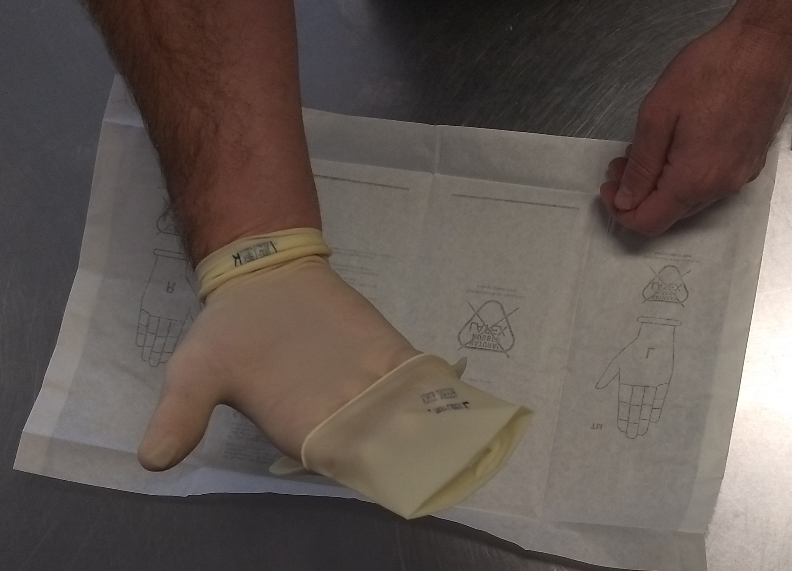
- Gloves
- Select the correct sized gloves. Ensure the gloves are pulled over the sleeve cuffs.
Sequence for removal (doffing) of PPE
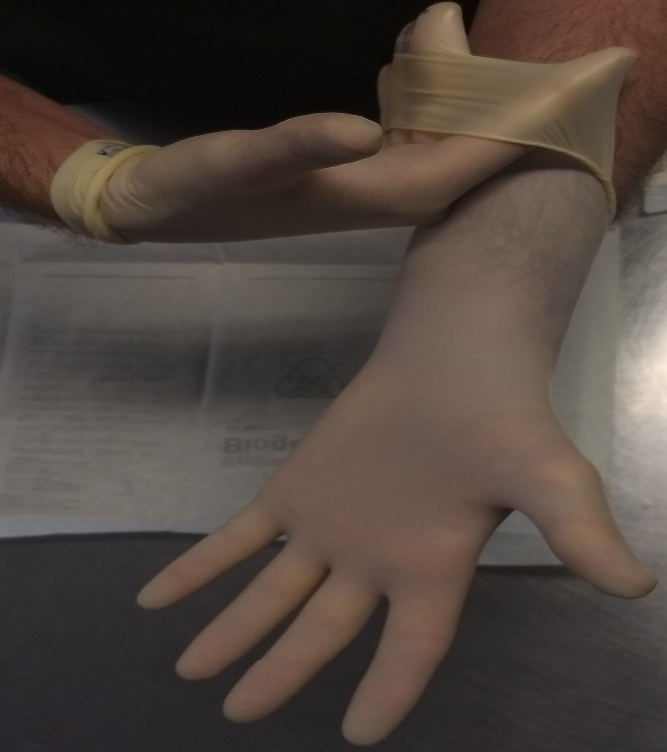
- Gloves
- Grasp outside of glove with opposite gloved hand and peel off.
- Hold removed glove in gloved hand.
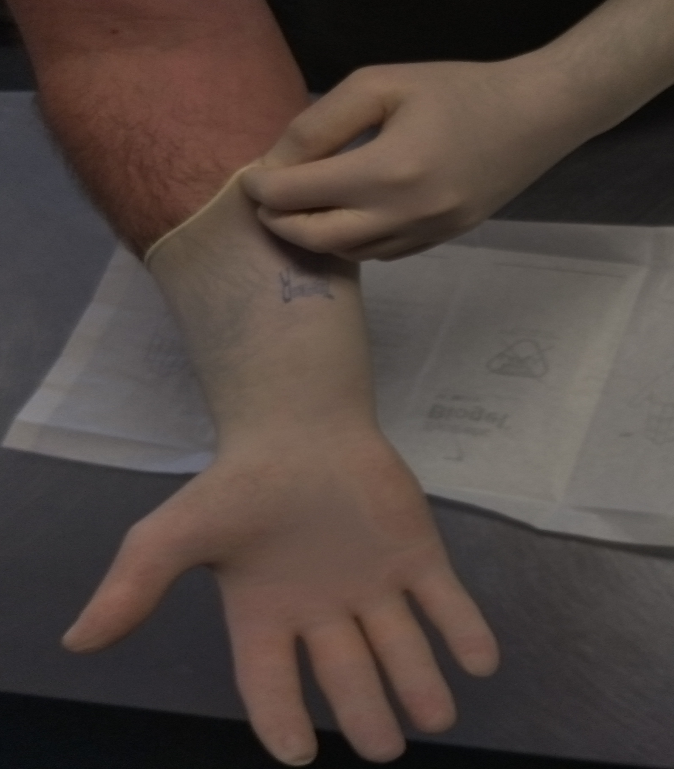
- Slide fingers of ungloved hand under the remaining glove at wrist.
- Peel glove off over the first glove and discard in waste bag.
- Perform hand hygiene
- Gown/Coveralls
- Gowns - Unfasten ties. Pull away from neck and shoulders, touching the inside of the gown only. Gown front and sleeves are likely to be contaminated. Carefully fold or roll into a bundle and place in waste bag
- Coveralls - Unzip suit and carefully remove. Roll outwards leaving non-contaminated inside exposed – assistance may be required from a colleague. Carefully fold up suit, and place in waste bag.
- Perform hand hygiene
- Protective Eyewear/face shield
- Remove protective eyewear or face shield by handling the ear pieces or headband – avoid touching the front of the eyewear/face shield as this is likely to be contaminated.
- Reusable eye protection can be cleaned and disinfected. Single use face shields to be disposed in waste bag.
- Perform hand hygiene
- P2/N95 respirator
- Remove respirator –do not touch the front of the respirator. Handle by the head straps and dispose in waste bag.
- Perform Hand hygiene
WA Health (2022) Respiratory Protection Guidelines for Western Australian Healthcare Facilities. Communicable Diseases Control Directorate.
National Health & Medical Research Council and the Australian Commission on Safety and Quality in Healthcare. (2021). Australian guidelines for the prevention and control of infection in healthcare. Canberra, Australia: Commonwealth of Australia.
Standards Australia/Standards New Zealand. AS/NZS 4011:1997/Amdt 1:1998. Single-use examination gloves - Specification. Sydney, Australia: Standards Australia International Limited.
Standards Australia. AS 4381:2015 Single-use face masks for use in healthcare. Sydney, Australia: Standards Australia International Limited.
Standards Australia/Standards New Zealand. AS/NZS 1716:2012. Respiratory protective devices. Sydney, Australia: Standards Australia International Limited.
Standards Australia/Standards New Zealand. AS/NZS 1715:2009. Selection, use and maintenance of respiratory protective devices. Sydney, Australia: Standards Australia International Limited.
Standards Australia/Standards New Zealand. AS/NZS 1336:2014. Recommended practices for occupational eye protection. Sydney, Australia: Standards Australia International Limited.
Standards Australia/Standards New Zealand. AS/NZS 1337:2010. Eye protectors for industrial application. Sydney, Australia: Standards Australia International Limited.
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.