
- To provide ventilatory support to apnoeic patients or those with insufficient respiratory effort to enhance oxygenation. Examples include:
- Cardio-respiratory arrest,
- Respiratory arrest, or
- Who have ineffective respiratory effort and are able to tolerate it.
Different Types of BVM
SMART BVM's and / or AMBU BVMs may both be available; this guidance is as generic as possible.
- Facial hair can affect seal, utilise KY jelly on areas were mask is to be seated.
- Be mindful of ventilation rate and pressure:
- Excessive ventilation pressure usually results in gastric distention and may compromise patency.
- Ventilating large volumes at high pressure with a mask will result in gastric distension and risk of regurgitation.
- If an i-gel®/ETT is in-situ, excess pressures in the thorax can be generated, impeding blood flow and can precipitate lung injury.
- Gentle ventilation at lower pressure will mitigate this. Some BVM’s may have built-in valves to prevent this.
- Tidal volume is usually approx 7mL/kg – this is hard to judge with BVM. Aim for chest rise but avoid excessive rise.
- Inability to ventilate indicates possible airway obstruction
- Patients less than 10kg should not spontaneously breathe through the BVM, due to possible suffocation.
- AMBU Bag BVM - The ‘pop off’ valve (if fitted) should remain in the open position when used in paediatric, infant and newborn patients. In some instances where higher airway pressures might be required such as upper airway obstruction, consideration could be given to close the pop-off valve, if there is an inability to ventilate. This should be a cautious decision.
- SMART-Bag BVM - In cardiac arrest, the flow restrictor should be engaged to avoid over-ventilation. This can be disengaged if the patient requires higher tidal volumes. The timing light should also be activated as a guide to prompt each adult inflation at 6 secs (~ after every 10th compression)
- Cricoid pressure is de-emphasised.
- Asthmatics and COPD patients require assisted ventilations at a lower ventilation rate of 4-6 breaths/min to allow better exhalation.
- Newborn patients should be ventilated with air initially; premature newborn should be ventilated with blended air – BVM at 1 L/min as per Newborn Life Support CPG.
- Do not ventilate against effective spontaneous efforts - attach SpO2 monitoring. Discontinue oxygenation through SMART BVM if saturations fail to rise >88% despite
- All relevant infection control methods to be utilised.
- Position the patient as necessary
- Prepare equipment required:
- Bacterial filter MUST be attached in patients > 20kg (bacterial filter is contraindicated where patient weight is < 20kg)
- Ensure the BVM is functional; seal the mask connecter with your hand and depress the bag to ensure there are no leaks.
Note: In cardiac arrest, compressions MUST NOT be interrupted for more than 2-3 secs to facilitate ventilation. Work as a team.
- Adjust oxygen flow rate to 15 litres per minute and allow the reservoir bag to fill completely before and between ventilations.
- Place patient in the most optimal position.
- Place the apex of the mask over the bridge of the patient’s nose, and then seal the mask over the patient’s chin. Open airway with jaw thrust and chin lift.
- Utilise the 'anaesthetist grip' to ensure a firm seal of the mask on the patient’s face.
- Reposition as required.
- Ventilate the patient as necessary; avoid hyperventilation and/or hyperinflation.
- In asynchronous CPR, the inflation MUST occur on the decompression phase (~after every 10th compression)
- Place patient in supine position.
- Continuously ensure the patient’s airway is patent, use suction if required, apply essential airway management and progress to advanced airway techniques if required.
- Attach BVM oxygen tubing to fir-tree port on O2 cylinder and turn regulator knob to ensure the reservoir bag inflates fully.
- Create an effective seal between the BVM and the face.
- Use an inverted hand at the end of the bag to avoid excess volume and pressure
- SMART BVM - The flow limiter is on the neck of the BVM, it should be engaged to limit pressure and volume in cardiac arrest
- Gently compress the bag to ventilate the patient. These can be timed with spontaneous breaths if necessary.
- Gauge the effort required to ventilate through the feel of the recoil bag to achieve minimal rise and fall of the chest. Excess pressure and volume is detrimental to the patient.
- The following ventilation rates are a guide for normal respiration values. DO NOT EXCEED.
- Do NOT provide asynchronous ventilation in paediatrics
| Newborn | 40 - 60 breaths per minute |
| < 1 year | 30 - 40 breaths per minute |
| 1 - 2 years | 25 - 35 breaths per minute |
| 2 - 5 years | 25 - 30 breaths per minute |
| 6 - 12 years | 20 - 25 breaths per minute |
| > 12 years | 15 - 20 breaths per minute |
| Adult | 10 - 12 breaths per minute |
- If patient is not breathing at an effective rate, assisted ventilations are to be performed.
- BVM resuscitator kit volumes:
| Neonate | 240 mL |
| Paediatric | 500 mL |
| Adult | 1600 mL |
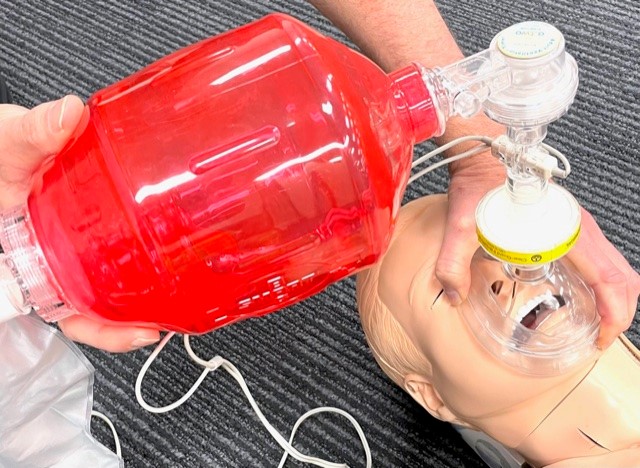
"Anaesthetist Grip"

Adult and combined Paediatric / Infant SMART BVM
Successful ventilation of a patient can be confirmed by factors such as:
- Rise and fall of chest
- Auscultation of lung bases and apexes, with air movement throughout
- Rise in oxygen saturation (SpO2)
- Reduction of cyanosis
- Waveform capnography
If bag is tight, consider and address:
- Poor patient positioining
- Asthmatic hyperinflation
- Tension pneumothorax
- Airway obstruction
- Impeded blood flow in cardiac arrest
- Abdominal distension and regurgitation
- Aspiration
- Barotrauma and lung injury
- Timing asynchronous inflation perfectly with decompression phases of CPR
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.