- To assist in the safe delivery of a baby.
- Prepare for Neonatal resuscitation
- All relevant infection control methods to be utilised.
- Consider vehicle for back-up.
- Prepare equipment required:
- Adult and infant BVM
- Baby mucus extractor & bacterial filter
- Oxygen
- Plastic bag
- Small combine
- Space blanket
- Sterile gauze pad
- Sterile scissors
- Towel
- Umbilical clamps
- Incontinence sheets
- Reassure mother, remove constrictive clothing and place an incontinence sheet below pelvis.
- Place in position of comfort.
- Administer high flow oxygen if indicated.
- Insert IV cannula if clinically indicated
- Consider appropriate analgesia.
Delivery of the child
- Identify if delivery is imminent by evidence of crowning[1], contractions 2-3 minutes apart or an urge to push.
- Coach mother to breathe deeply to relax between contractions and push with contractions.
- Be mindful of maternal faecal matter; only wipe away if at risk of soiling foetal airway (pressure placed on the mothers anus during childbirth can result in activation of pelvic floor muscles and delay the birth).
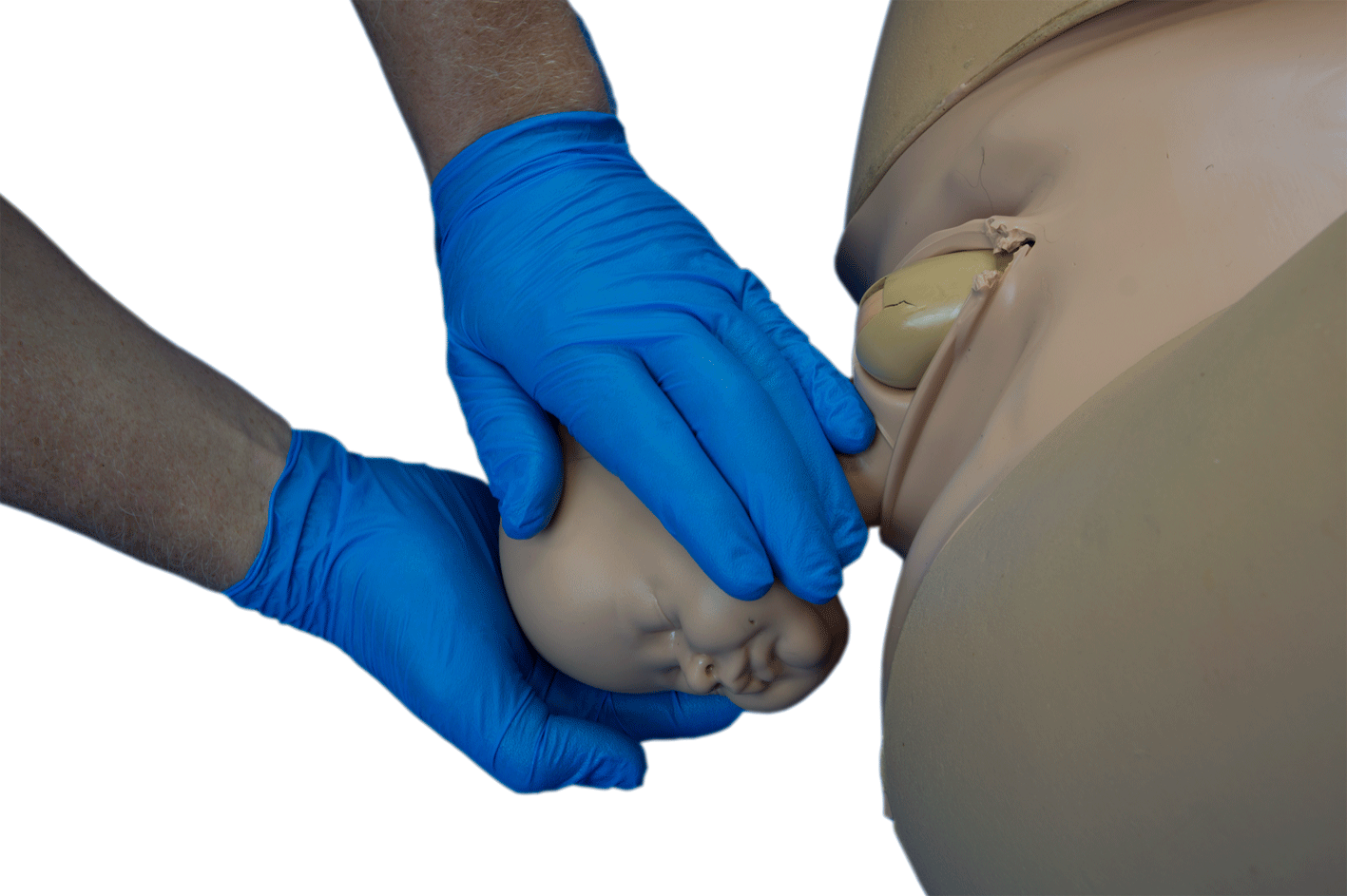
- As the baby’s head delivers provide support with one hand to prevent rapid delivery, spreading fingers to evenly distribute pressure on fontanels.
- Use the other hand to support the perineum with a dressing pad.
- Once the head is delivered, perform a visual check of the back of the head and neck to ensure cord is not wrapped around neck.
- If cord is present around neck and loose slide the cord over the baby’s head prior to the next contraction. Only if it is too tight and preventing the birth of the body, place two clamps on the cord approximately 3cms apart and cut between the clamps.
- Guide the baby’s head downwards to deliver the upper shoulder and then gently guide the head upwards to deliver the lower shoulder while supporting the baby[2].
- Allow the baby to deliver itself without pulling.
- Only suction the mouth and nose of the newborn using the Penguin Suction Device to ensure airway cleared if required.
- Stimulate baby to induce crying, e.g. rubbing with towel on back.
- The cord does not need to be cut in the prehospital setting, unless the baby or mother requires immediate intervention. Delayed cord clamping is encouraged, maximum benefits have been achieved by 3-4 minutes.
- Should immediate intervention be required, make best effort to keep cord intact. If not possible due to environmental constraints, clamp and cut the umbilical cord with two cord clamps. Place the first clamp 4 fingers from the baby’s body, place the second clamp 2 fingers further away from the baby away and cut between the 2 clamps. If bleeding persists on either end, apply a third clamp.
- If the umbilical cord has been ruptured or torn, the cord must be clamped as a priority to prevent neonate volume loss. This is to be done regardless of if there is visible blood loss from the cord
- Record delivery time, second officer to perform APGAR (3) and care for newborn.
| Sign | 0 Points | 1 Point | 2 Points | |
|---|---|---|---|---|
| A | Appearance (Skin Colour) | Blue-gray, pale all over | Normal, except for extremities | Normal over entire body |
| P | Pulse | Absent | Below 100 bpm | Above 100 bpm |
| G | Grimace (Reflex Irritability) | No Response | Grimace | Sneeze, cough, pulls away |
| A | Activity (Muscle Tone) | Absent | Arms and Legs Flexed | Active Movement |
| R | Respiration | Absent | Slow, irregular | Good, crying |
Placenta Delivery
- Skin to skin contact and the suckling of the newborn will induce the delivery of the placenta. The mother will experience the same contractions as with delivery of the baby.
- Prepare a Bio-hazard bag to place the placenta into when delivered.
- Do not pull on cord.
- The placenta may take up to 60 minutes after the delivery of the baby to be expelled.
- Ensure the placenta is taken with the mother to hospital.
Care of the Mother
- Apply pad to vagina post delivery, and ensure no excessive blood loss has occurred.
- Instruct mother to keep pad in place by keeping legs closed.
- Remove the soiled linen from under buttocks and wipe off any fluids from mother’s legs.
- Cover mother and keep warm.
- Monitor mother and baby en route to hospital.
- Record APGAR at 1, 5 and 10 minutes.
Potential complications:
- Bleeding prior to delivery
- Cord prolapse
- Malpresentation
- Placenta previa
- Postpartum haemorrhage
- Premature birth
- Shoulder dystocia
- Cord rupture
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.