
- Assessment and treatment of minor skin tears, abrasions and lacerations.
- Significant wounds meeting anatomical criteria of Major Trauma Guidelines
- Time critical patients
- Significant burns requiring large dressings
| Key aseptic terms for minor wound care | |
|---|---|
| Key sites: | Wound |
| Key parts: | Dressing, tweezers |
- Always take a full history, specifically identifying if patient is taking any anti-coagulation medications (eg. Warfarin, Aspirin etc). This will delay clotting times and may predispose patient to unidentified bleeds (especially in head injuries). Also consider patients taking steroids or other immunosuppressive medications as this may affect wound healing and mask signs of infection.
- Identify and document the mechanism of injury, including any contributing factors such as neurological or cardiac causes.
- Treatment of wounds is a procedure that has the potential to expose the patient to infection. Always utilise aseptic technique to mitigate infection risk to patient.
- Avoid performing wound care in proximity of potential contaminants. This may require removal of patient from surroundings to maintain a sterile field.
- Consider if patient is appropriate for Uncomplicated Wound Care Pathway
- Any injury that occurs whilst in care of St John WA must be documented and logged as a Clinical Incident.
- Elderly patients are at particular risk of skin tears during patient movement procedures, such as transferring from stretcher to bed.
- Consider consultation of Falls Prevention Guideline for elderly patients to determine risk of falls causing injury.
- Utilise Trauma Management Principles as required and consider Major Trauma Guidelines
Gain patient consent:
- Explain procedure to patient and gain consent where applicable. Note this may require informing the patient of the requirement to move to a more appropriate location
Assess the patient:
- Assess for wound type (laceration, abrasion, skin tear). Document size and location of wound, and type of skin tear if applicable.
- Perform hand hygiene
- Assess and, if necessary, control any haemorrhage
- Assess neurovascular observations distal to injury, document if any compromise
- Consider use of cophenylcaine if indicated
- Determine cause of injury
- Assess wound and determine if any requirement for wound cleaning or irrigation
Prepare the equipment:
- Perform Hand Hygiene
- If using sterile dressing pack:
- Clear/clean area suitable to place dressing pack
- Appropriately sized non-adherent dressing that will cover wound.
- 2 x 10mL sterile Sodium Chloride 0.9% (if wound irrigation required. If not, only 1 needed)
- Appropriately sized crepe bandage
- 10mL syringe
- Open dressing pack with the tips of your fingers and spread out on clean work surface.
- Draw up Sodium Chloride 0.9% into 10mL syringe for irrigation
- Pour 10mL Sodium Chloride 0.9% into appropriate area on dressing tray.
- Open dressing and place on to dressing pack without touching dressing
- Using sterile tweezers, place non-woven dressings into Sodium Chloride 0.9%
- If not using sterile dressing pack:
- Clear/clean area suitable to place clean absorbent pad
- Appropriately sized non-adherent dressing that will cover wound
- Appropriately sized crepe bandage
- 2 x 10mL sterile Sodium Chloride 0.9% (if wound irrigation required. If not, only 1 needed)
- 10mL syringe (if wound irrigation is required)
- If wound irrigation required, draw up 10mL of Sodium Chloride 0.9% into 10mL syringe
Procedure:
- Consider use of analgesia prior to performing procedure
- Place clean absorbent pad underneath wound site if required.
- Perform hand hygiene
- Don all relevant PPE
- Irrigation:
- Utilising drawn up Sodium Chloride 0.9% in 10mL syringe, irrigate wound with gentle pressure to clear foreign body from site. Be mindful of potential for splash.
- If using sterile dressing pack:
- If skin tear present:
- Using sterile tweezers, place skin flap back across wound as anatomically correct as possible, however do not force into place.
- Using sterile tweezers place non-adherent dressing on to wound.
- Utilising aseptic technique, use gentle pressure to keep dressing in place whilst covering dressing site with crepe bandage.
- If skin tear present:
- If sterile dressing pack unavailable:
- Open dressing without touching dressing
- Moisten dressing with sterile Sodium Chloride 0.9%
- Only touching the edges of the dressing, place the dressing on the wound. DO NOT TOUCH THE DRESSING WHERE IT WILL MEET THE WOUND
- Utilising aseptic technique, use gentle pressure to keep dressing in place whilst covering dressing site with crepe bandage
- Assess distal neurovascular observations. If there is change, reassess crepe bandage tightness and adjust if required.
- If bleeding recommences and there is noticeable bleeding through the dressing, place a combine on top of the crepe bandage. Do not remove the initial dressing.
- Wound is dressed appropriately with no signs of continued bleeding
- Distal neurovascular observations are not compromised post application of dressing
- If bleeding recommences apply dressing on top of in place dressing
- If changes to distal neurovascular observations adjust dressing as required. This may require re-application of dressing
SJWA Minor Wound Referral Pathways
Please follow the link below to determine if your patient is eligible to be referred to an alternate care pathway.
| Minor wound definition chart | |
|---|---|
| Skin tear |
|
| Abrasion |
|
| Laceration |
|
| Signs and symptoms of wound infection | |||
|---|---|---|---|
| Wound type | Localised infection | Spreading infection | Systemic infection |
| Acute wound |
| As per localised infection plus:
|
|
| Chronic wound |
|
|
|
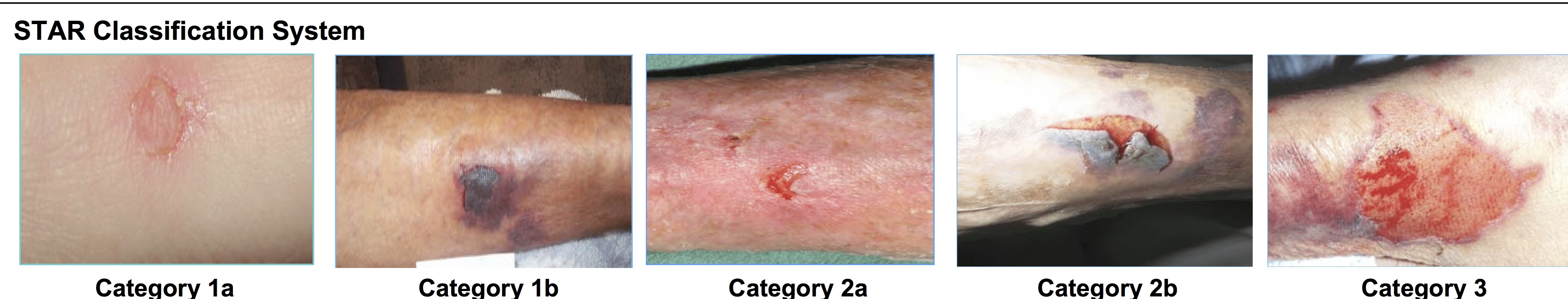
| Skin Tear Audit Research (STAR): Skin Tear Assessment Tool | ||||
|---|---|---|---|---|
| Category 1A | Category 1B | Category 2A | Category 2B | Category 3 |
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Barr N, Mason M, Clegg L, Randall F. Maintaining asepsis in paramedicine: a Delphi study: Asepsis in paramedicine. Australas j paramed . 2022;19. Available from: https://ajp.paramedics.org/index.php/ajp/article/view/954
Unsworth J, Collins J. Performing an aseptic technique in a community setting: fact or fiction? Prim Health Care Res Dev. 2011;12(1):42–51. Available from: https://www.cambridge.org/core/journals/primary-health-care-research-and-development/article/performing-an-aseptic-technique-in-a-community-setting-fact-or-fiction/FE590986EF818149DA7B3F0EBF5B173F
Sonoiki T, Young J, Alexis O. Challenges faced by nurses in complying with aseptic non-touch technique principles during wound care: a review. Br J Nurs. 2020;29(5):S28–35. Available from: http://dx.doi.org/10.12968/bjon.2020.29.5.S28
Australian Commission on Safety and Quality in Healthcare. NSQHS Standards Implementation guide for Action 3.11 Aseptic Technique. December 2022. https://www.safetyandquality.gov.au/sites/default/files/2022-01/nsqhs_standards_implementation_guide_for_action_3.11_aseptic_technique_-_december_2021.pdf
Silver Chain Nursing Association and Curtin University of Technology School of Nursing and Midwifery. STAR Skin Tear Classification System. February 2010.
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.