- To minimise complications during transportation of a potential breech birth and facilitate delivery only when inevitable.
- Patient is male
- Cord prolapse (7.4%)
- Foetal head entrapment in (0-8.5%)
- Perinatal mortality
- Postpartum haemorrhage
- Premature placental separation
- Prolonged compression of cord
- Trauma:
- Brachial plexus
- Brain/skull
- Fractured humerus, femur or clavicle
- All relevant infection control methods to be utilised.
- Prepare equipment required:
- Adult and infant BVM
- Baby mucus extractor
- Oxygen
- Placenta bucket
- Small combine
- Space blanket
- Sterile gauze pad
- Sterile scissors
- Towel
- Umbilical clamps
- Place in the lithotomy position[1] and move buttocks to end of bed.
- Administer high flow oxygen.
- Insert IV cannula.
- Consider appropriate analgesia.
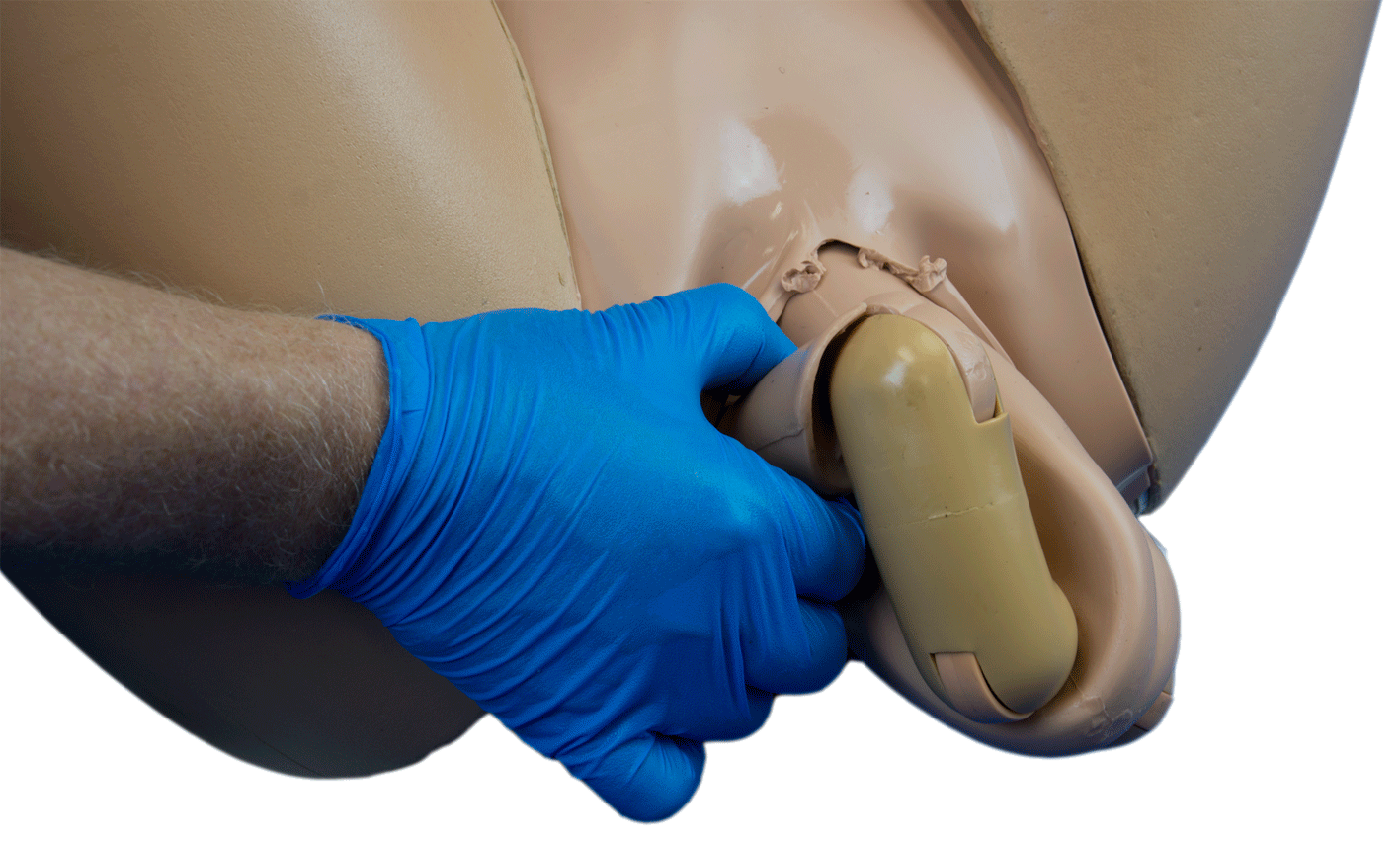
- If foetus’ buttocks are presenting[2] on the perineum encourage the mother to actively push during contractions.
- Allow the legs, abdomen and trunk to deliver by maternal effort. Once the buttock is born external rotation of buttocks is seen whereby the baby’s back becomes uppermost[3].
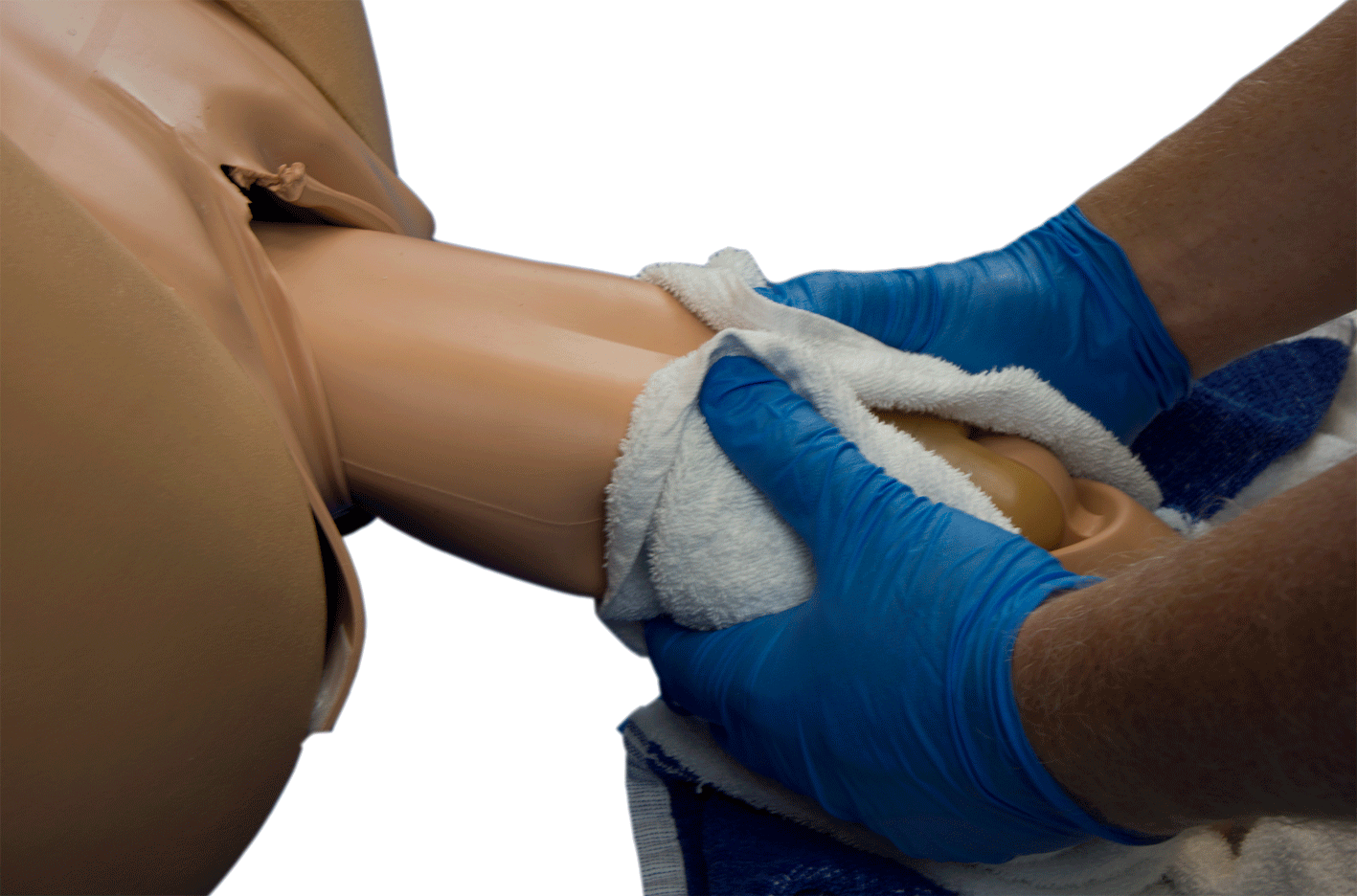
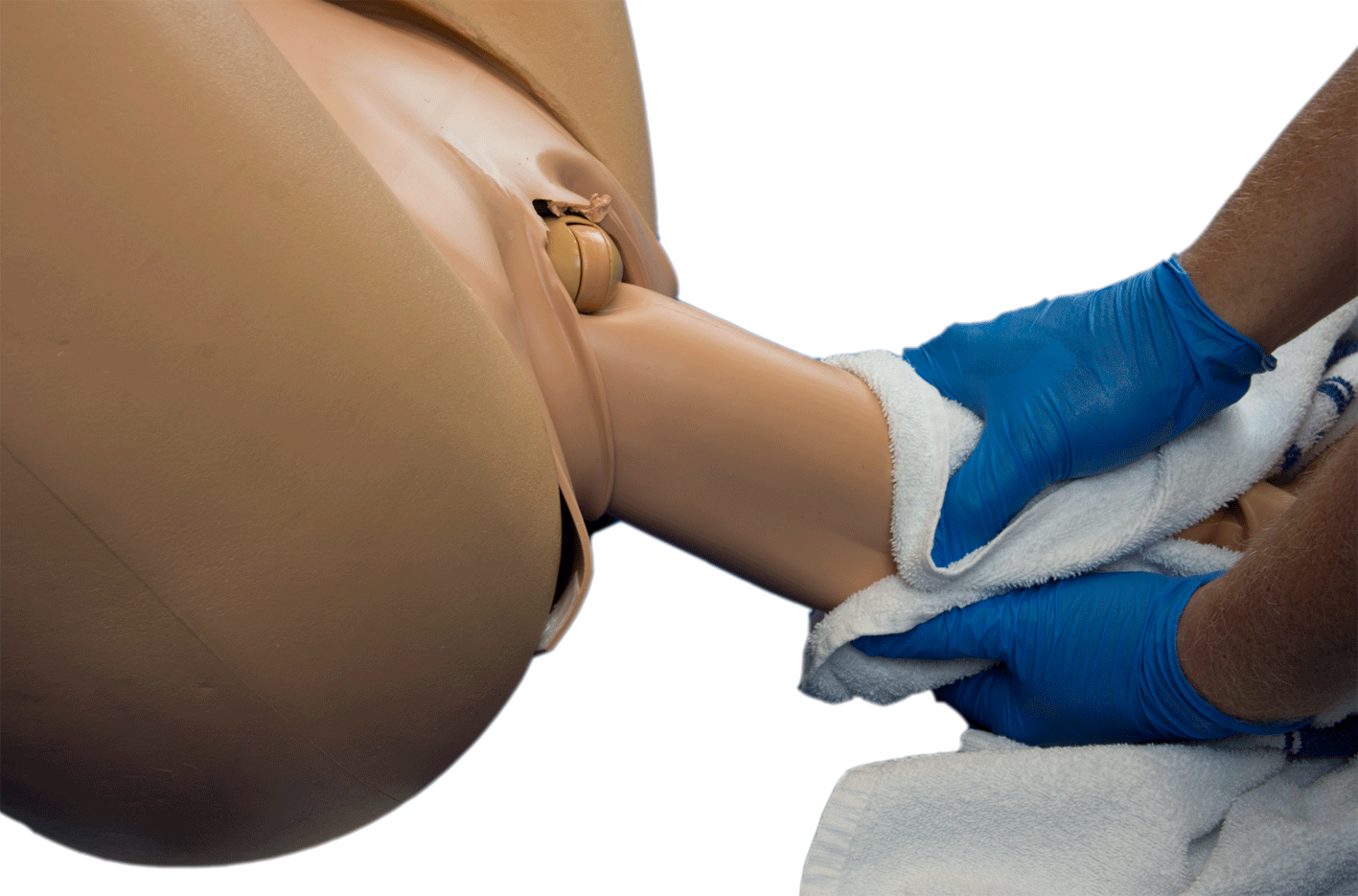
- If legs are extended slide two fingers along the anterior leg and apply gentle pressure in the popliteal fossa.
- Deliver the legs by flexion and abduction[4].
- Gently bring down a loose loop of cord (approximately 15cm).
- If the shoulders do not spontaneously deliver place a single layer towel over the hips and buttocks and grasp the pelvic girdle with thumbs on the sacrum and index and mid fingers on the hips[5].
- Once the tip of the scapula comes into view gently rotate the posterior shoulder anteriorly into the oblique by rotating the baby through 180°. The sacrum is kept anterior at all times.
- With the next contraction and maternal effort apply gentle downward traction to deliver the shoulder[6].
- Gently rotate through 180° in the opposite direction to bring the anterior shoulder into the other oblique plane.
- Deliver the anterior shoulder by using gentle downward traction. Keep the sacrum anterior.
- If an arm is extended and obstructs progress slide two fingers along the anterior arm and apply gentle pressure in the cubical fossa. Flex the arm and swept across the chest and out of the vagina. Rotate the baby to original position with back facing uppermost.
- Place forearm under the baby for support.
- Commence delivery of the head with the next contraction. Maintain foetal head in a flexed position to allow passage.
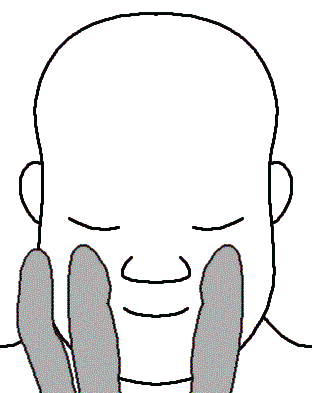
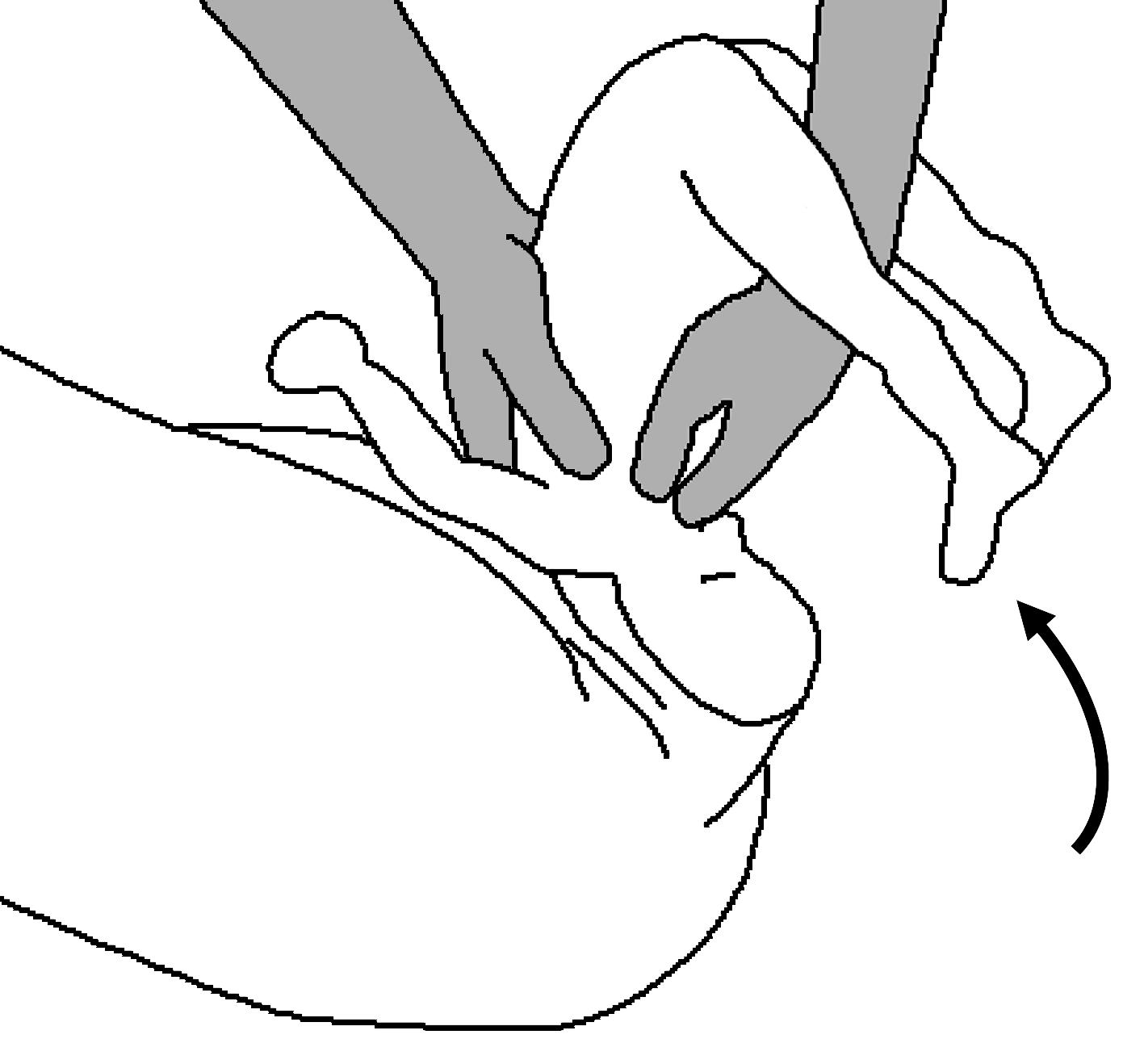
- Perform Mauriceau Smellie Veit manoeuvre: place index and middle fingers on the foetal maxillary prominences[7], raise upwards[8]
- Note and record time of birth.
- Proceed with normal neonatal care.
- If the baby’s head does not deliver within 3 minutes transport the mother in an exaggerated Simms position[9]. Apply a V hold on the baby’s face if practical[7].
- Maintain a warm environmental temperature using blankets/towels.
- Advise receiving hospital.
- Monitor and record mother’s blood loss.
Frank

Complete

Footling

- Continue with Childbirth clinical skill.
- If the baby’s head does not deliver within 3 minutes, transport the mother Priority 1 to the nearest obstetric hospital in an exaggerated Simms position[9].
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.