- Advanced airway management is the assessment and protection of a compromised airway via the use of techniques such as patient positioning, suction, oropharyngeal, supraglottic and surgical airway (Cricothyrotomy).
- Endotracheal intubation is de-emphasised and should not occur un-necessarily
- A Vortex-like approach should be utilised for a considered and structured management approach in:
- Cardiac arrest patients
- Patients with an unprotected airway that has risk of compromise:
- A-reflexic patients with a GCS ≤8, especially head trauma, without a gag reflex
- Induction (CCP Only)
- In the vast majority of cases, a supraglottic airway device is adequate and simple troubleshooting approaches can mitigate problems (e.g. avoidance of high pressure ventilations that cause cuff leak).
- An absolute need for endotracheal intubation is very infrequent
- Officer managing airway is to control all patient movements.
- Adjunct placement, ventilation efficacy and capnography waveform must be re-assessed following all patient movements.
The most competent, current and appropriate clinician in relation to airway management should manage/coordinate the process:
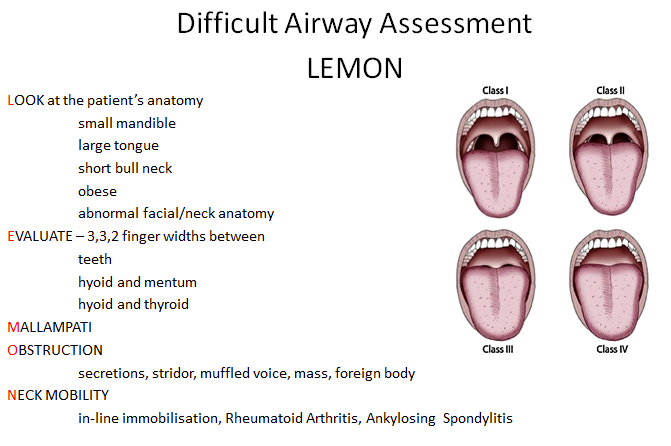
Airway assessment (LEMON)
- L - Look externally
- E - evaluate 3:3:2
- M - mallampati airway difficulty grade 1-4
- O - obstructions
- Suction
- Magill Forceps
- N - neck mobility (query spinal injury)
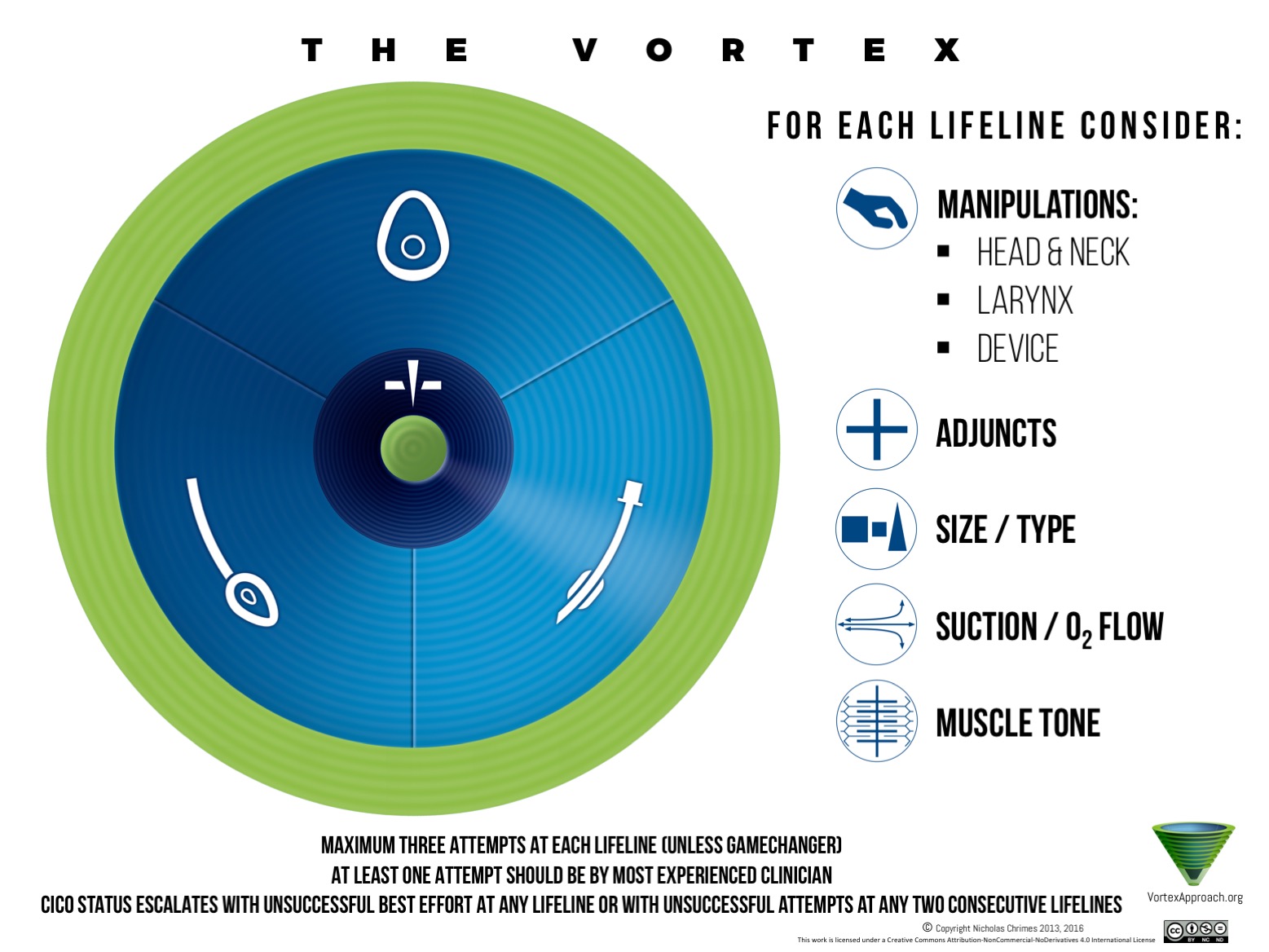
Vortex approach to airway management:
- Patient positioning
- Adjuncts oropharyngeal (OPA) or nasopharyngeal (NPA) airway
- BVM with rise and fall of chest
- Supraglottic Airway
If this fails to provide ventilation then:
- Intubation if absolutely necessary and authorised
- Surgical Cricothyrotomy (vertical)
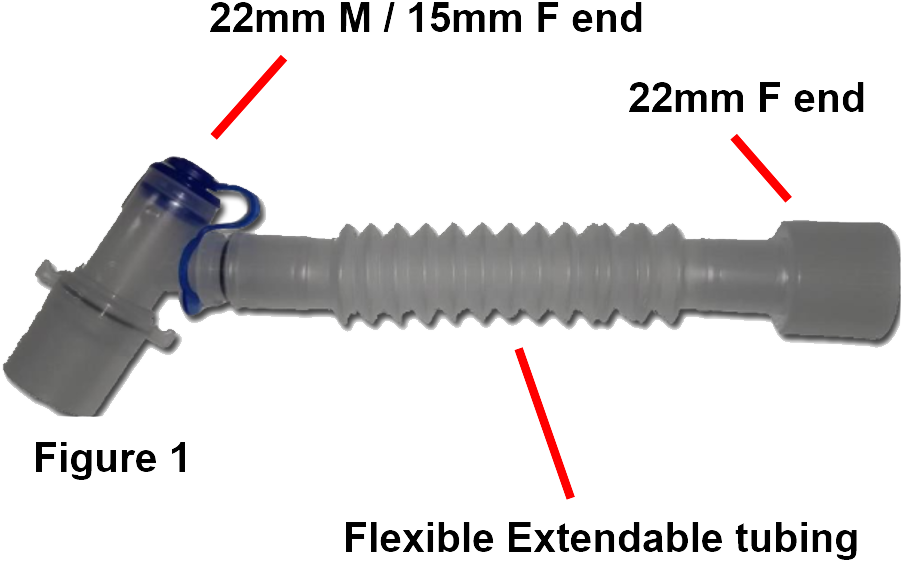
Disposable Catheter Mounts
- Catheter Mounts can be used to add ‘extra length’ and flexibility to the breathing circuit when needed.
- Catheter Mounts are connected as an intermediary between the airway adjunct and the BVM.
- The catheter mount is made of flexible co-polymer and has a double swivel connector and flexible tubing as this provides mobility and flexibility to the patient end of the circuit.
- The length of the tubing is around 13 cm. Be aware it increases dead space.
- The Catheter Mount also comprises of a suction port and cap.
- Remove from packaging, extend and connect to adjunct
- If suctioning is required, open the cap on the suction port and directly insert flexible suction tubing to a depth no more than the length of the airway adjunct
- When suctioning is no longer required, secure the cap over the suction port
Perform ventilation assessment and document checks:
- ETT Only:
- Visualised ETT passing through vocal cords
- Misting of tube
- Adequate rise and fall of chest
- Auscultation of epigastric area first and subsequently both left and right lungs.
- End tidal CO2 waveform and reading in mmHg
- Laryngeal spasm
- Displacement during patient movements/transfer; care should be taken, i.e. disconnect the BVM when moving patients, re-assess after moves, see notes above.
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.