
- RSI is a high-risk procedure in the prehospital environment and is currently undertaken by single-operator CCPs
- Reported complication rate in ED is around 40% and serious hypoxia in up to 22% of intubations, which is associated with increased morbidity and mortality1.
- Preoxygenation allows a safety buffer during periods of hypoventilation and apnoea, which, in critically unwell patients is often poorly tolerated2.
- In this setting, the risk of hypoxia outweighs the risk of gastric aspiration and therefore avoidance of ventilation during the apnoea phase may be detrimental 3. This is an alternative to human delivered bag-valve mask ventilations which frequently result in excessive ventilation that increase risk of gastric insufflation and aspiration.
- It has been designed to provide a maximum positive inspiratory pressure of 15cm H2O. It is thought that the lower oesophageal sphincter is unlikely to allow gastric insufflation below pressures of 20cm H2O. By this rationale it is expected to allow safe ventilations during the apnoea period where traditionally in Rapid Sequence Intubation the patient receives no external ventilation.
- Studies have shown that in critically hypoxic patients, use of NIV as a preoxygenation technique leads to higher mean SpO2 prior to intubation and maintenance of higher SpO2 levels during intubation4. No negative cardiovascular effects or appreciable gastric distension were noted 5,6.
- Ventilator-assisted preoxygenation (VAPOX) in patients who remain hypoxic on high flow O2
- The use of NIV for preoxygenation should be observed in patients who cannot achieve acceptable saturations with high flow 02 via non-rebreather mask (>93%)
- If intubation is attempted with saturations below 90%, these patients can critically desaturate in seconds7.
- If this is required as a method of preoxygenation then it may be of benefit to have them on this device until the moment of intubation, as PEEP also prevents absorption atelectasis caused by breathing high Fi02, increasing the efficacy of apnoeic oxygenation 8. (see table 1)
- Facial Trauma or deformity
- Upper airway obstruction
Table 1: Risk categorization of patients during preoxygenation
Risk Category Based on pulse oximetry whilst receiving high flow oxygen | Preoxygenation Period (3 minutes) | Onset of muscle relaxation (~ 60 seconds) | Apnoeic period (Variable duration dependent on airway difficulty, ideally <30 seconds) |
|---|---|---|---|
| Low risk (SpO2 96-100%) |
|
|
|
| High risk (SpO2 91-95%) |
|
|
|
| HYPOXAEMIC (SpO2 <91%) |
|
|
|
- This patient group should receive preoxygenation in a head-elevated position wherever possible (minimum ~ 20 degree head elevation)
- For potential spinal injury patients, reverse Trendelenberg position can be used (figure 1)
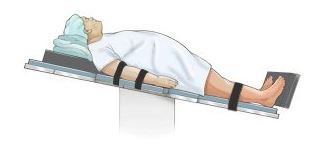
Figure 1: reverse Trendelenberg positioning
- Turn Hamilton T1 Ventilator on to NIV-ST mode with the following settings:
- RR 6-8 breaths/min
- Pinsp 10mmH20
- PEEP 5cmH20
- O2 100%
- ETS (expiratory trigger sensitivity) 50%
- Inspiratory flow trigger 2L/min
- Ti: 2seconds
- P-ramp 50ms
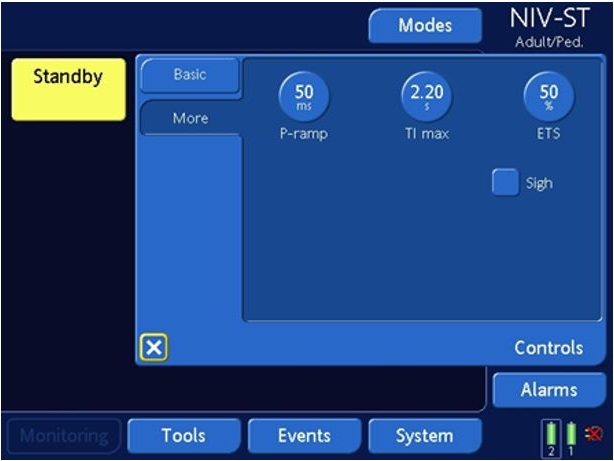
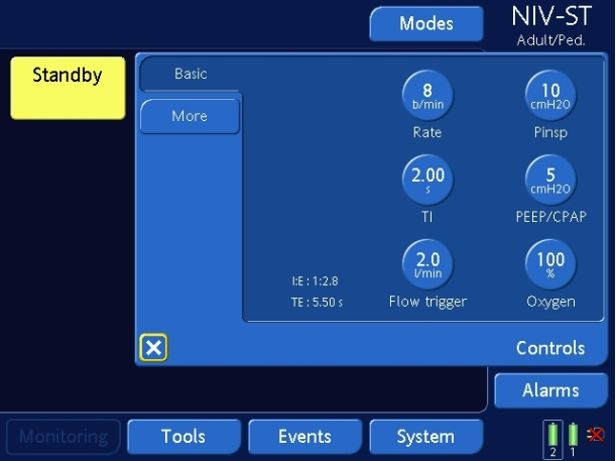
Figure 2: Hamilton T1 Ventilator settings for VAPOX
- Place NP on patient but do not turn on 02 at this point
- Size NIV mask (from bridge of nose to crease between bottom lip and chin – see below)

- Place mask on patients face and secure straps ensuring no obvious leaks
- Insert Etc02 between mask and flow sensor
- Titrate PEEP between 5-15cmH20 to achieve Sp02 >98%
- Allow patient to breathe at tidal volume for 3 minutes
- Agitated or combative patients may require small aliquots of ketamine to tolerate the process (titrate up to 1mg/kg)
- Push sedative and paralytic
- Leave NIV mask in situ for this period (it will transition to PCV+ once apnoea ensues)
- Turn NP 02 on to 15L/min
- Leave high flow NP in situ throughout intubation period to maintain apnoeic oxygenation
| Settings | |
|---|---|
| Extended Care: | |
| Colour assist: | |
Simpson GD, Ross MJ, McKeown DW, Ray DC. 2012. Tracheal intubation in the critically ill: a multi-centre national study of practice and complications. Br J Anaesth; 108:792-9
Farmery AD, Roe PG. 1996. A model to describe the rate of oxyhaemoglobin desaturation during apnoea. Br J Anaesth; 76:284-91
Grant S, Khan F et al. 2016. Ventilator-assisted preoxygenation: Protocol for combining non-invasive ventilation and apnoeic oxygenation using a portable ventilator. EMJ; 28:67-72
Baillard C, Fosse JP Sebbane M et al. 2006. Noninvasive ventilation improves preoxygenation before intubation of hypoxic patients. Am J Respir Crit Care Med; 174:171-77
Cressey DM, Berthoud MC, Reilly CS. 2001. Effectiveness of continuous positive airway pressure to enhance pre-oxygenation in morbidly obese women. Anaesthesia; 56:680-684
Jaber S, Jung B, Corne P et al. 2010. An intervention to decrease complications related to endotracheal intubation in the intensive care unit: a prospective, multi-centre study. Intensive Care Med; 36:248-255
Weingart S, Levitan RM. 2012. Preoxygenation and Prevention of Desaturation During Emergency Airway Management. Annals of Emergency Medicine; 59:165-75
Rothen HU, Sporre B, Engberg G et al. 1995. Prevention of atelectasis during general anaesthesia. Lancet; 345: 1533-1543
Document Control
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.