
Definition
Anaphylaxis is any acute onset of hypotension, bronchospasm or upper airway obstruction where anaphylaxis is considered possible. Even if typical skin features are not present OR any acute onset illness with typical skin features (urticarial rash or erythema/flushing
and/or angioedema) PLUS involvement of respiratory and/or cardiovascular and/or persistent severe gastrointestinal symptoms.
Epidemiology
Anaphylaxis is generally under-reported and many unexplained deaths could be anaphylaxis. Statistically, the facts are difficult to collate due to various factors such as different hospital codes and the cause of death may not be specifically attributed to anaphylaxis, but natural causes.
Source: Australasian Society of Clinical Immunology and Allergy
Pathophysiology
Anaphylaxis the most severe form of an allergic reaction. Immediate allergic reactions are due to an interaction between Immunoglobulin-E (IgE) antibodies and an antigen (allergen) with a resulting release of chemicals from cells such as basophils and mast cells.
Review of a normal immune response (antigen/antibody reaction):
- Antigen:
- Substances (usually a protein) that enter your body and induce the formation of antibodies. These may sometimes referred to as allergens. A substance that is an allergen for one person may not be for another.
- Substances (usually a protein) that enter your body and induce the formation of antibodies. These may sometimes referred to as allergens. A substance that is an allergen for one person may not be for another.
- Antibody:
- Neutralises antigens and removes them from the body.
- Immunoglobulin E (IgE):
- Accounts for less than 1% of antibodies in normal serum. Responsible for immediate hypersensitivity reactions
- Basophil:
- A white blood cell that promotes inflammation
- Mast cell:
- Distributed amongst connective tissues (skin, lungs, GI tract which is where allergens are mostly likely to enter the body) . Filled with vasoactive amines (histamine, serotonin, leukotrienes).
Mast cells release amines as part of the inflammatory response. They have a role in defending the body against parasites and they have receptors for IgE antibody on their surface.
This release is stimulated by antigens binding to IgE, injury (i.e. trauma) or chemical agents (e.g. toxins, or in some people, physical stresses such as exercise).
- Distributed amongst connective tissues (skin, lungs, GI tract which is where allergens are mostly likely to enter the body) . Filled with vasoactive amines (histamine, serotonin, leukotrienes).
Antigens may enter the body by:
- Injection
- Ingestion
- Inhalation
- Absorption
Antigens will enter the system and trigger an immune response which leads to the production of antibodies (or immunoglobulins) which are designed to fight the invading antigens by binding to them and causing degranulation of the cell. This degranulation will cause a release of the chemicals that will fight the invading cells, such as histamine.
This normal antigen– antibody reaction is what protects the body from disease by activating the immune response. The immune responses are normally protective, however they can become oversensitive and become directed toward harmless antigens to which we often are exposed; this response is known as an allergic response.
Mild to moderate allergic reactions
These reactions do not involve the circulatory or respiratory system. They usually occur minutes to 2 hours of exposure to an allergen.
Mild to moderate symptoms:
- Hives or welts
- Tingling mouth
- Angioedema (swelling of lips, face, eyes)
- Abdominal pain (this is a sign of anaphylaxis to medications and insect stings and bites)
- Vomiting (this is a sign of anaphylaxis to medications and insect stings and bites)
Treatment is typically with non-sedating antihistamines, which compete at the receptor sites with histamine. By doing so, this prevents histamine from performing its physiological actions. An antihistamine can help with the skin symptoms of an allergic reaction (like hives or swelling). They will not treat anaphylaxis.
Anaphylaxis
Anaphylaxis is usually rapidly progressing and is an acute hypersensitivity reaction that can affect multiple organ systems. It is a severe life threatening event which may impact one or more of the cardiovascular or respiratory systems.
Anaphylaxis is caused by the widespread release of inflammatory mediators which results in a systemic increase in capillary permeability, smooth muscle contractility and peripheral vasodilation. Allergic sensitisation occurs when an antigen enters the body and activates the immune system response, leading to the production of IgE antibodies directed against that antigen. These antibodies then remain inactive on the cells until another exposure to the antigen and are referred to as antigen specific immunoglobulins.
When the antigen enters the body again, it binds to the IgE antibodies on mast cells and basophils. This interaction causes degranulation of the cell and the release of chemical mediators to fight the allergen.
These chemical mediators include:
- histamines
- leukotrienes
- heparin
- kinins
- prostaglandins
- thromboxanes
The effects of these chemical mediators include:
- An increase in the permeability of vessels
- Causes dilation of capillaries and venules (causing flushing & angioedema)
- Plasma leaks into interstitial space (decreases intravascular fluid volume and causes swelling)
- Vasodilation further decreases cardiac preload, decreasing stroke volume and cardiac output (hypotension)
- Contraction of smooth muscle in the GI tract and bronchial tree (associated with increases in gastric, nasal and lacrimal secretions and bronchospasm)
Because the body sees the allergen as dangerous, it tries to protect the body from this perceived invader, just as it would a harmful parasite. Antihistamines do not prevent or treat anaphylaxis as they don’t work against all the mediators and they don’t work immediately. Adrenaline reverses most of the effects listed above and it works within minutes so it is the treatment of choice for anaphylaxis.
Causes
Common causes of anaphylaxis are:
- Medications (e.g. antibiotics such as penicillin)
- Food (e.g., peanuts, tree nuts, cow’s milk, egg, wheat, fish, shellfish, sesame, soy (note; any food can induce anaphylaxis))
- Envenomation (bee, wasp and ant stings, tick bites)
- Latex
- In some people, physical stresses (e.g. exercise (with or without prior food ingestion) or immersion in cold water) can lead to an anaphylaxis like reaction.
- Some people may have idiopathic anaphylaxis (no cause identified)
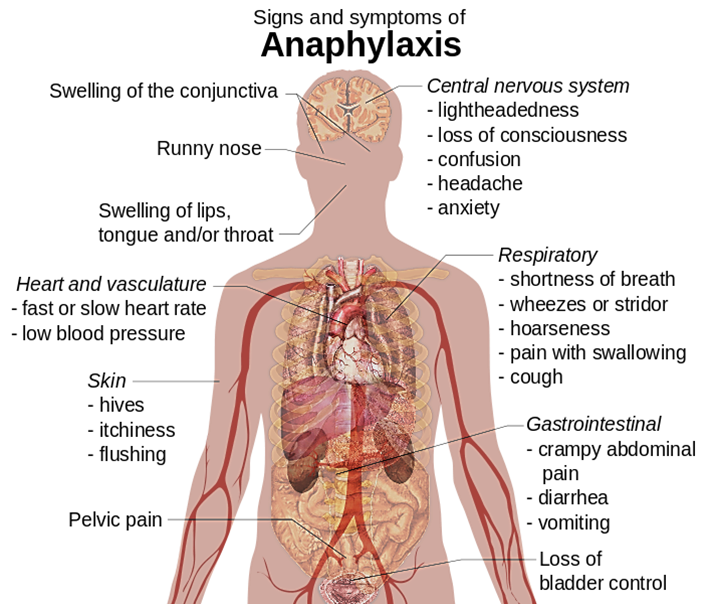
Signs and Symptoms
Symptom onset depends on the route of exposure:
- Injection: Average onset 5 to 30 minutes
- Ingestion: Within minutes, and may take up to 2 hours
Anaphylaxis is characterised by any one or more of the following (typically rapidly developing) symptoms:
- Difficult/noisy breathing.
- Swelling of tongue
- Swelling/tightness in throat
- Difficulty talking and/or hoarse voice
- Wheeze or persistent cough.
- Persistent dizziness and/or collapse
- Change of consciousness
- Hypotension
- Pale and floppy (young children)
Complications
Anaphylactic Shock
- Inadequate tissue perfusion due to, widespread vasodilation and increased vascular permeability leading to reduced cardiac output and cardiac failure secondary to an allergic response
Page contributors:
 | Default Author St John WA |
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.