
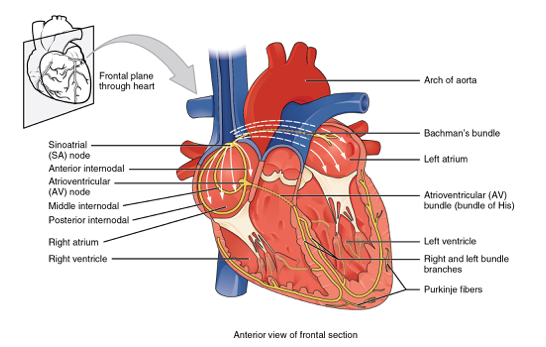
Observe the Atrioventricular (AV) Node in the upper-mid portion of the heart, and the Left and Right Bundle Branches at the intraventricular septum
Heart block type that originate from a group of arrythmias raised from failed or delayed transmission above the atrioventricular (AV) node to the ventricles - Classified into 1st, 2nd & 3rd degree AV blocks.
- If QRS is < 0.12s then the AV block is located in AV node or Bundle of His (better prognosis)
- Broad QRS indicates distal blocks (further than bifurcation of Bundle of His)
- Conduction system degrading or ischemia
- Idiopathic Fibrosis of conduction system
- Vagal stimulation
- Hyperkalaemia
- Medications (Beta Blockers, Digoxin, Amiodarone, Verapamil etc.)
- Lyme Disease (Borreliosis)
- Hypothermia
| Type of AV block | Definition | Clinical Features |
|---|---|---|
| 1st Degree AV block | Difficulty transmitting impulse through AV node (where SA node is normal). | Due to this delay, the PR interval is longer – Once this travels through AV node, the impulse travels normally. |
| 2nd Degree AV Block / Mobitz-Type I (Wenchkebach) | Represents a delayed transmission impulse through the AV node – However the time it takes to reach the ventricles increase for every impulse. | This results in gradual PR interval increase. This continues until SA node intervenes with a sinus beats which resets the cycle again to prevent a fall in blood pressure. The RR interval shortens with each beat of the cycle. The P-P interval remains constant |
| 2nd Degree AV block / Mobitz-Type II | Severe 2nd degree block resulting in a dropped beat, due to SA node impulse not being transmitted to the ventricles. | If 2 or more impulses are blocked at the AV node before reaching the ventricles, it is called 2:1 or 3:2 block. Can develop into 3rd degree AV block or ventricular standstill. |
| 3rd Degree AV block / Complete Heart Block | No communication through AV node resulting in separate atrial & ventricle transmission by their own branches. The SA node fires at 60-100 where the ventricles are at about 20-40bpm from nearby impulses from AV node or; within the ventricles. | Perfusion is through junctional or ventricular escape rhythm – Can result to ventricle standstill. Hypotension is displayed due to inability of atria to intervene resulting in diminished cardiac output. |
Normal PQRST wave means good normal conduction – Conduction is initiated by the sinoatrial node (SA node) in the right atrium.
- Impulse spread to left atrium via Bachmann Bundles and towards ventricles via AV node
- In the ventricles, impulse travel along Bundle of His then
- The impulse then bifurcates (divide) into left & right bundle branches
- These branches terminate in a network of conduction tissues (Purkinje Fibres)
Conduction is very fast – In event where conduction branch is impaired, the impulse finds a way past the obstruction by transmitting impulses from cell-to-cell until it can re-join the fast conduction system again. Hence the process is delayed (due to added time due to added distance as result of the blockage) reflected by a wider QRS complex.
Examine QRS width & configuration for right (V1 / V2) & left (V5 / V6) ventricles
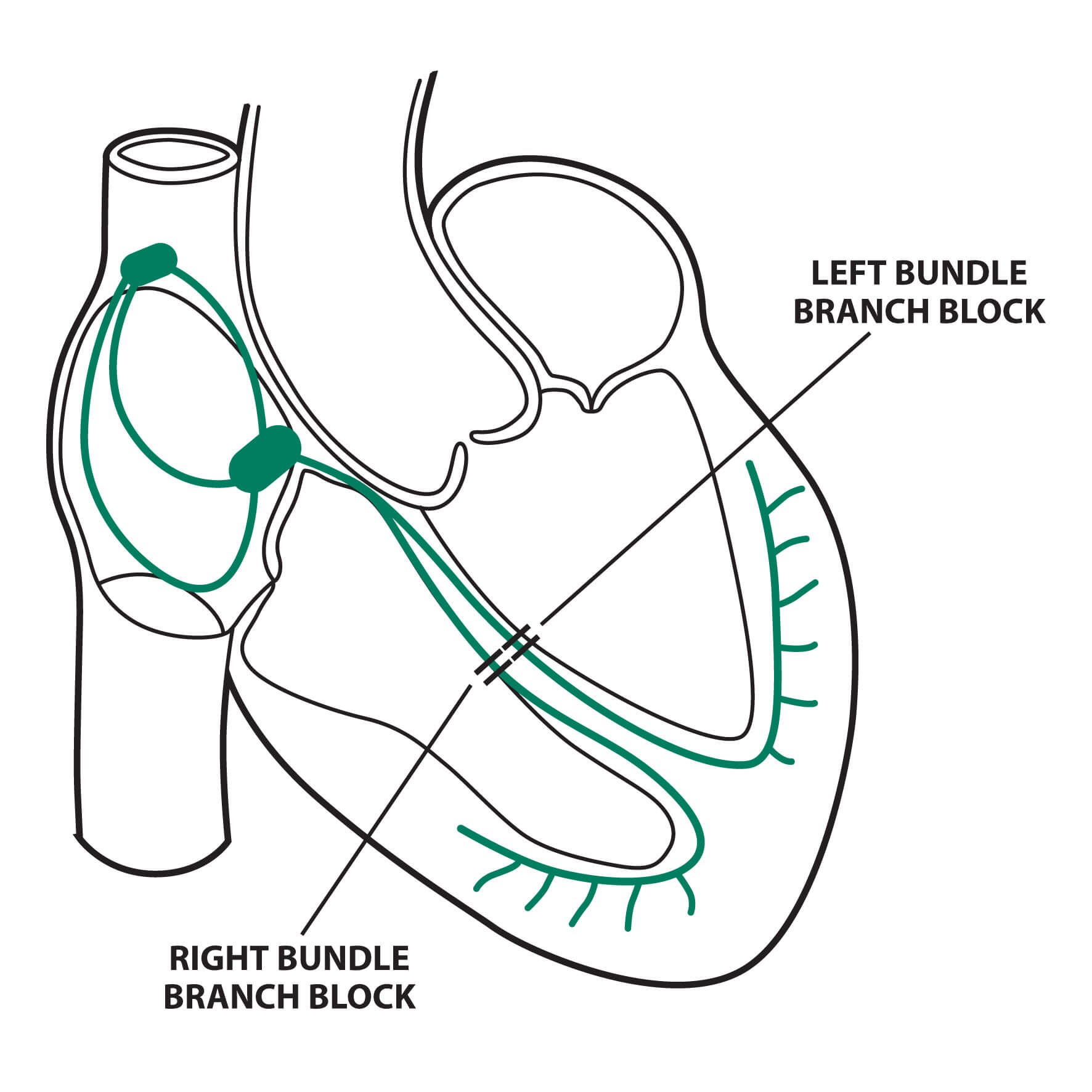
- When there is a conduction delay (widened QRS) without LBBB or RBBB – Can be observed after a large MI event where necrotic areas can cause conduction disturbances – Some other changes can be due to myocardial fibrosis, amyloidosis, cardiomyopathy or hypertrophy.
- 1. > 110 ms (2.5 to 3 small boxes or more) in adults OR;
- 2. > 90ms (2 to 2.5 small boxes or more) in children 8 to 16 years OR;
- 3. > 80ms (2 small boxes or more) in children < 8 years AND;
- 4. Do not met criteria for RBBB or LBBB.
- When the conduction through the right bundle is obstructed (delaying right ventricular depolarisation) – Depolarisation of right ventricle will rely on the impulse from the left ventricle.
- QRS complex > 0.10 (wide)
- rSR’ / rsr’ / rsR’ complex pattern in V1 & V2
- Second R-wave (R’) is larger than 1st R-wave and S-waves does not reach the baseline – Basically QRS displays “M” shape.
- ST depression & T-wave inversion in V1 & V2
- Deep & Broad S-Wave in Lead I, aVL, V5-V6
- Secondary ST-T changes (ST-T segment opposite to QRS)
TIP: Compare V1 & V6
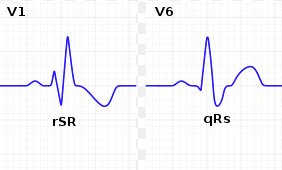
- V1 produces an “M” shape pattern
- V6 has a broad & deeper S wave
Example 1:
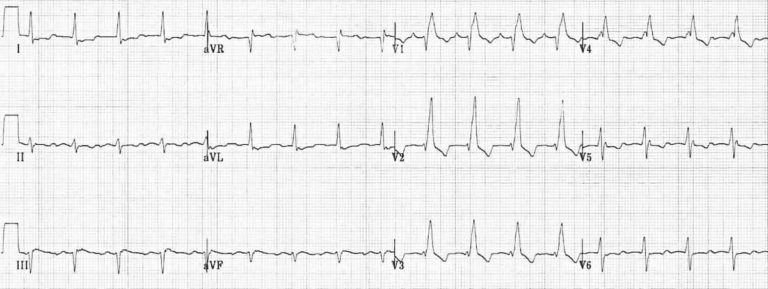
Example 2:
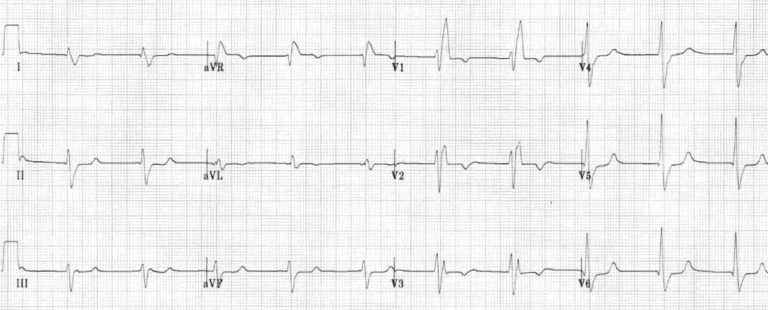
The impulse from left ventricle will be slow as it needs to travel partly or entirely outside of the conduction system resulting in slow & abnormal activation of right ventricles creating an abnormal and prolonged QRS complex. Therefore, the left ventricle will activate before the right ventricle; therefore, displaying its own vector.
- Idiopathic fibrosis or RBB degeneration
- Heart disease
- Coronary Artery Disease
- Pulmonary Embolism
- COPD
- Cardiac surgery or PCI may cause RBBB
- Cardiomyopathy
- When the conduction through the left bundle is obstructed (delaying left ventricular depolarisation) – Depolarisation of left ventricle will rely on the impulse from the right ventricle.
- QRS complex > 0.10 (wide)
- Lateral QRS has a broad / notched R-wave with prolonged upstroke in Lead I, aVL, V5-V6
- ST depression & T-wave inversion in Lead I, aVL, V5-V6
- V1 & V2 has asymmetrical, broad, & deep QS complexes.
- V1-V3 may have ST elevation (< 5mm) & positive T-waves
- Left axis deviation may be present (due to dominant ventricle)
TIP: Compare V1 & V6
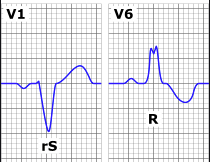
- V1 produces rS wave (V-shape QRS)
- V6 mini ‘M’ on the peak of QRS
Example 1:
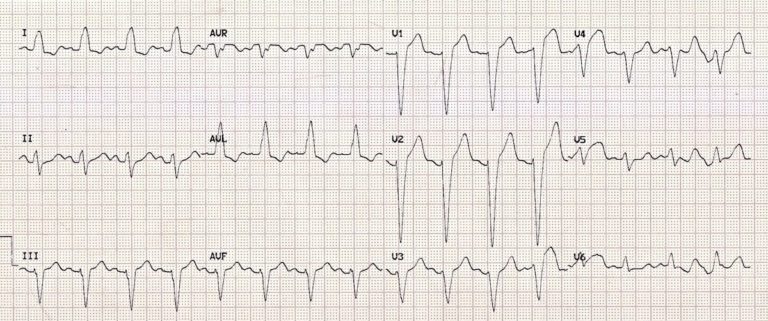
Example 2:
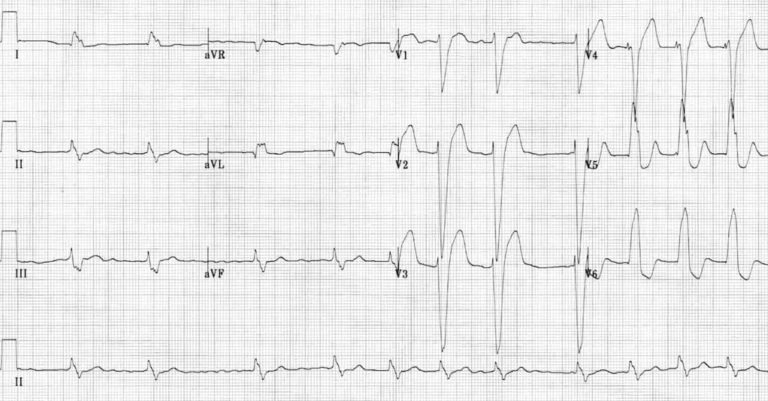
The impulse from right ventricle will be slow as it needs to travel partly or entirely outside of the conduction system resulting in slow & abnormal activation of left ventricles creating an abnormal and prolonged QRS complex.
- Ischemia & infarction (may be masked by LBBB)
- Idiopathic fibrosis or LBB degeneration
- Heart disease
- Coronary Artery Disease
- Cardiomyopathy
Left bundle branch contains three (3) fascicular left, right and septal branch – Hemiblock is a block to one (1) fascicular branch only, therefore is not a complete LBBB. A normal conduction is when the impulse move down AV node to left bundle, then split into both fascicles where the Purkinje fibres merge - A hemiblock rely on impulses from other parts of the ventricles where fascicle is intact.
- Can occur in healthy individuals, or those suffering from conditions such as LBBB related symptoms, or ventricle hypertrophy, & medications. Can be progressive to other blocks but rare.
Due to the block, the impulse backtracks and move down to the left posterior fascicle (LPF) causing left axis deviation.
- Can mask symptoms of anteroseptal infarction
- rS complex in Lead II, III, & aVF can mask Q-wave from prior inferior infarction
- QRS 0.10 – 0.12s in V5 & V6
- Left axis deviation (-60°)
- No other cause of LBBB
- Larger branch (greater blood supply); due to the block, the impulse backtracks and move down to the left anterior fascicle causing right axis deviation – similar causes as left anterior fascicular block (LAFB; unusual in healthy people, and overall rare)
- Can mask inferior & lateral infarction
- T-wave inversion may occur in inferior leads showing similar to post-ischemic T-wave
- QRS 0.10 – 0.12s in V5 & V6
- Left axis deviation (+120°)
- No other cause of LBBB
- No right ventricle hypertrophy
Bifascicular Block
Combination of either left anterior or left posterior hemiblock with RBBB – Dangerous condition as only one fascicle of left bundle branch is supplying the heart with electrical activity.
- RBBB present
- Left axis deviation or right axis deviation present
Page contributors:
 | Thanh Bui, AP60825 Event Medic, Emergency Medical Technician & Volunteer Development Officer
|
 | Andrew Moffat, AP16790 |
Clinical Resources Website
St John Ambulance Western Australia Ltd (ABN 55 028 468 715) (St John WA) operates ambulance and other pre-hospital clinical services. St John WA’s Clinical Resources, including its Clinical Practice Guidelines (Clinical Resources), are intended for use by credentialed St John WA staff and volunteers when providing clinical care to patients for or on behalf of St John WA, within the St John WA Clinical Governance Framework, and only to the extent of the clinician’s authority to practice.
Other users – Terms of Use
The content of the St John WA Clinical Resources is provided for information purposes only and is not intended to serve as health, medical or treatment advice. Any user of this website agrees to be bound by these Terms of Use in their use of the Clinical Resources.
St John WA does not represent or warrant (whether express, implied, statutory, or otherwise) that the content of the Clinical Resources is accurate, reliable, up-to-date, complete or that the information contained is suitable for your needs or for any particular purpose. You are responsible for assessing whether the information is accurate, reliable, up-to-date, authentic, relevant, or complete and where appropriate, seek independent professional advice.
St John WA expressly prohibits use of these Clinical Resources to guide clinical care of patients by organisations external to St John WA, except where these organisations have been directly engaged by St John WA to provide services. Any use of the Clinical Resources, with St John WA approval, must attribute St John WA as the creator of the Clinical Resources and include the copyright notice and (where reasonably practicable) provide a URL/hyperlink to the St John WA Clinical Resources website.
No permission or licence is granted to reproduce, make commercial use of, adapt, modify or create derivative works from these Clinical Resources. For permissions beyond the scope of these Terms of Use, including a commercial licence, please contact medservices@stjohnambulance.com.au
Where links are provided to resources on external websites, St John WA:
- Gives no assurances about the quality, accuracy or relevance of material on any linked site;
- Accepts no legal responsibility regarding the accuracy and reliability of external material; and
- Does not endorse any material, associated organisation, product or service on other sites.
Your use of any external website is governed by the terms of that website, including any authorisation, requirement or licence for use of the material on that website.
To the maximum extent permitted by law, St John WA excludes liability (including liability in negligence) for any direct, special, indirect, incidental, consequential, punitive, exemplary or other loss, cost, damage or expense arising out of, or in connection with, use or reliance on the Clinical Resources (including without limitation any interference with or damage to a user’s computer, device, software or data occurring in connection with such use).
Cookies
Please read this cookie policy carefully before using Clinical Resources from St John WA.
The cookies used on this site are small and completely anonymous pieces of information and are stored on your computer or mobile device. The data that the cookies contain identify your user preferences (such as your preferred text size, scope / skill level preference and Colour Assist mode, among other user settings) so that they can be recalled the next time that you visit a page within Clinical Resources. These cookies are necessary to offer you the best and most efficient possible experience when accessing and navigating through our website and using its features. These cookies do not collect or send analytical information back to St John WA.
Clinical Resources does integrate with Google Analytics and any cookies associated with this service enable us (and third-party services) to collect aggregated data for statistical purposes on how our visitors use this website. These cookies do not contain personal information such as names and email addresses and are used to help us improve your user experience of the website.
If you want to restrict or block the cookies that are set by our website, you can do so through your browser setting. Alternatively, you can visit www.internetcookies.com, which contains comprehensive information on how to do this on a wide variety of browsers and devices. You will find general information about cookies and details on how to delete cookies from your device. If you have any questions about this policy or our use of cookies, please contact us.